
Medically Reviewed by Iga Gray, M.D. NVISION Surgeon
Medications for Glaucoma: Types, Side Effects & Effectiveness
Home / Diagnosed With Glaucoma /
Last Updated:

Medically Reviewed by Iga Gray, M.D. NVISION Surgeon

Article At a Glance
Glaucoma medications—most commonly in the form of eye drops—help lower eye pressure to prevent vision loss. This article explains the main types of medications, how they work, and when they’re prescribed. Some reduce fluid production in the eye, while others improve drainage. There are also combination drops and oral medications for more advanced cases. It’s important to follow your treatment plan exactly and discuss side effects with your doctor. If drops are hard to manage or not effective, alternative treatments like laser or surgical options may be recommended. Regular follow-ups help keep your vision protected.
Table of Contents
A few generations ago, a glaucoma diagnosis meant you were on a path to losing your eyesight. Thanks to modern technology and a better understanding of glaucoma, doctors today have much better tools to diagnose and manage glaucoma and prevent it from robbing you of your eyesight.
Common medications for glaucoma include eye drops and oral options. In this article, we’ll examine the types of popular glaucoma treatment options, their side effects, and the effectiveness of each in managing glaucoma.
A Brief Overview of Glaucoma
Glaucoma is a set of diseases that affect your optic nerve. Glaucoma causes excess pressure in the eye, known as intraocular pressure. At first, the condition seemingly has no symptoms. By the time symptoms begin to show, it is often too late and irreversible damage has already occurred. This is why regular eye exams are key to early diagnosis.
Fortunately, if you have been diagnosed with glaucoma, various medications and eye drops are available to treat the condition.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Eye Drops for Glaucoma
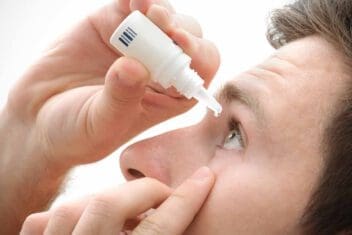
All glaucoma medications are meant to decrease pressure on the optic nerve. The goal is to preserve your vision for as long as possible.
Per the Glaucoma Research Foundation, glaucoma medication is classified by its main active ingredient. Each type has certain advantages and potential side effects. Here are a few of the most common drop-based medications for glaucoma:
Beta Blockers
These decrease pressure in the eye by reducing liquid production. Depending on progression, these may be used once or twice daily.
Examples include timolol (Istalol, Betimol, and Timoptic) and betaxolol (Betoptic).
Side effects include decreased blood pressure, lower heart rate, breathing difficulties, and fatigue.
Alpha-Adrenergic Agonists
These eye drops decrease the production of eye fluid and improve drainage in the eye. This class of eye drops may be used along with other types of eye drops. Alphagan P is a brand known to be better for people who have allergies to preservatives, which are found in other types of eye drops. You can expect to use this type of eye drop twice per day, though they are occasionally prescribed for use up to three times per day.
Examples include brimonidine (Qoliana, Alphagan P) and apraclonidine (Iopidine).
Side effects include dry mouth, increased blood pressure, increased heart rate, and red, swollen, or itchy eyes.
Carbonic Anhydrase Inhibitors
Also called CAIs, these eye drops tend to be used along with other types of eye drops. They are usually prescribed for use twice per day, but they may be prescribed for use three times per day. They reduce the amount of fluid your eye produces.
Examples include brinzolamide (Azopt) and dorzolamide (Trusopt).
Side effects include increased urination, a metallic taste, red eyes, eyelid reactions, a burning feeling, fatigue, changes to libido, and weight loss.
Prostaglandins
These reduce eye pressure by helping to fluid drain outward. Typically, prostaglandins are used once daily.
Examples include latanoprostene bunod (Vyzulta), bimatoprost (Lumigan), latanoprost (Xalatan), travoprost (Travatan Z), and tafluprost (Zioptan).
Side effects include blurry vision, eye redness, stinging sensations, darkening of the skin in or around the eyelids, eyelash growth, and darkening in or around the iris.
Cholinergic (miotic) Medications
These work by enabling the eye to better drain itself. These can be prescribed for use up to four times per day. Side effects for cholinergic medications can be severe, and these drops are not prescribed often as a result.
Examples include Pilopine, Isopto Carbachol, and Isopto Carpine.
Side effects include pupil constriction that makes it hard to see in darker areas, such as movie theaters, as well as blurry vision, eye aches, and headaches.
Side Effects of Glaucoma Medications
Many of these eye drops for glaucoma can cause some serious side effects. This is because the medication in these eye drops is absorbed by the bloodstream. Closing the eyes for a minute or two after using these drops can reduce the possibility of absorption to the rest of the bloodstream.
If you have to use more than one of these medications, wait about five minutes between using each type. Generally, patients will use eye drops for as long as their doctor finds them necessary.
It can be tough to remember to use your eye drops as prescribed. Many patients do not get the full benefits of their medication because they forget to use it. If you are concerned about being able to remember and adhere to your drops schedule, ask your ophthalmologist about iDose TR, the newest treatment for glaucoma. It eliminates the need to remember daily doses or worry about missed applications, making it easier to maintain stable eye pressure at all times.
Oral Medications for Glaucoma

Eye drops may not always effectively manage glaucoma on their own. Oral medications can help glaucoma patients, but they should be used with caution. Their side effects may include:
- Metallic taste.
- Depletion of potassium.
- Kidney stones, in rare cases.
Oral carbonic anhydrase inhibitors (CAIs) were once the standard of care until eye drops and topical treatments became the most popular way to manage glaucoma symptoms. Neptazane (methazolamide) and Diamox (acetazolamide) are two of the CAIs that were once a standard part of glaucoma treatment protocol.
They are known to effectively decrease intraocular pressure, but their use is only recommended:
- For people who must wait a while to schedule surgery but need to manage symptoms in the interim.
- For people who cannot have surgery due to medical complications or are not willing to have one.
- As a first step during a laser procedure.
- When CAI eye drops cannot be taken.
- To prevent pressure from increasing after cataract surgery.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Are There Any Medications I Should Avoid?
Glaucoma medication can help you manage the condition and preserve your eyesight. Oral medication may be a great temporary solution for people who have to wait to get surgery. Eye drops can help to manage symptoms.
The potential side effects of these medications should be considered. Your doctor will ask you about supplements, herbal remedies, and medications you are currently taking, and instruct you on possible interactions.
Grapefruit is known to interact with many common medications. Data is still needed to understand whether or not it poses problems for people taking glaucoma medicine, but it is a good idea to ask your doctor about grapefruit consumption if you are prescribed medications to treat glaucoma.
Over-the-counter medications that dilate the pupils should not be taken if you have open-angle glaucoma. They could cause you to develop angle-closure glaucoma. These include the following:
- Antihistamines
- Decongestants
- Medication for motion sickness
- Certain antidepressants
As always, talk to your doctor about any other medications you are taking.
Sticking with Eye Drops
To avoid permanent vision loss, you should use your glaucoma eye drops every day as prescribed by your doctor. Some patients tend to skip their daily eye pressure drops multiple times during recovery or, worse, stop using their prescription altogether.
A study by Wilmer Glaucoma Center of Excellence found out that:
- On average, each glaucoma patient uses only 70 percent of their prescription eye drops
- About 25 percent of patients given a new prescription for glaucoma eye drops never refill their medication
- Only 50 percent of patients who refill their eye drops at least once stick to their dosage to the end of the first year
Skipping or stopping using your glaucoma eye drops allows the disorder to worsen. With your eye pressure out of control, irreversible optic nerve damage continues. The habit could eventually cause permanent blindness in the affected eye.
Here some tips to help you remember using your prescribed dose of glaucoma eye drops every day:
- Practice taking your medication at the same time as a daily routine like breakfast
- Use a smartphone, tablet, or smartwatch pill reminder app to track your doses and get timely prescription refill alerts
- If you have any memory issues, you may ask a family member to remind you
If you are concerned about remembering to take your glaucoma drops regularly, ask your doctor about iDose TR, the newest treatment for glaucoma. iDose TR provides continuous, around-the-clock medication adherence. This 24/7 adherence eliminates the need to remember daily doses or worry about missed applications, making it easier to maintain stable eye pressure at all times.
Frequently Asked Questions
What kinds of treatments can I expect if I’m diagnosed with glaucoma?
Eye drops and oral medication are both available and commonly used to treat glaucoma. With both types of medications, the goal is to reduce pressure on the optic nerve and preserve eyesight.
Eye drops work by either reducing the production of liquid in the eye or allowing liquid to drain from the eye faster. They are available as beta blockers, CAIs, prostaglandins, alpha-adrenergic agonists, and cholinergic eye drops. Oral CAIs are also available if eye drops are not controlling the problem.
Are there any side effects associated with glaucoma medications?
Yes, eye drops and oral medication can cause side effects.
Eye drops may cause redness, stinging or burning sensations, eyelash growth, changes to the color of skin around the eyelid, darkening of the iris, dry mouth, a rise in blood pressure, changes in heart rate, blurry vision, difficulty seeing in dark spaces, headaches, and eye aches. Not everyone will feel the same side effects, and not all eye drops will cause the same symptoms.
Oral CAIs are known for causing side effects that are more systemic in nature, meaning they will affect other organ systems. They can cause persistent side effects, such as a metallic taste in the mouth, kidney stones, and potassium depletion.
What if I’m taking supplements or medication for another condition?
Your doctor will note any medications you are currently taking and warn you about possible interactions. Be aware that you should avoid over-the-counter medication that causes pupil dilation, such as decongestants, antihistamines, and anything that helps with motion sickness. Certain antidepressants can also pose problems for people who are undergoing glaucoma treatment.
Will I need to take glaucoma medication forever?
Provided that your glaucoma drugs prescribed to you are working, you’ll probably need to use them every day for the rest of your life. If you experience any serious side effects, contact your ophthalmologist before halting your medication. It’s likely that your doctor will change your prescription or lower the dosage on your current medication to alleviate the adverse effects you see and feel.
Is there a better way to treat glaucoma besides medication
Glaucoma can also be controlled surgically, including as a first-line treatment plan.
The main types of surgeries to treat the eye condition are:
- Laser surgery: The procedure eases eye pressure by enhancing the drainage of fluid from the eye.
- Drainage implant surgery: Your surgeon may insert a small tube in your eye to drain fluid into a special reservoir.
- Cataract surgery: With this procedure, your eye’s lens is extracted to reduce pressure on the optic nerve.
Some patients start glaucoma treatment with drugs but later go on to have surgery. Most of them require this procedure if their initial medication fails to work or causes severe complications.
But: You are likely to need certain glaucoma drugs even after surgery.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Glaucoma. Kellogg Eye Center, Michigan Medicine.
- Glaucoma Medications and Their Side Effects. (July 2018). Glaucoma Research Foundation.
- Glaucoma Treatment. (August 2019). American Academy of Ophthalmology.
- Medication Guide. (July 2016). Glaucoma Research Foundation.
- Don’t Let Glaucoma Steal Your Sight! (December 2018). Centers for Disease Control and Prevention.
- Glaucoma Medicines. (January 2019). National Eye Institute.
- Eye Drop Tips. (October 2017). Glaucoma Research Foundation.
- Oral CAIs: Still An Option Worth Using. (April 2006). Review of Ophthalmology.
- Closed Angle Glaucoma: Angles to Avoid. (December 2017). Cigna.
- Grapefruit and Some Drugs Do Not Mix. (July 2017). Food & Drug Administration.
- Which Medications Treat Glaucoma? WebMD.
- An Eye on Glaucoma Drugs. (August 2018). Harvard Health Publishing.
- How to Succeed at Eye Drop Treatment: It’s All In Your Hands. Glaucoma Center of Excellence.
- What is Glaucoma? (September 2021). American Academy of Ophthalmology.

Dr. Iga N. Gray is a comprehensive ophthalmologist with a specialization in glaucoma, currently practicing at Alvarado Eye Associates in San Diego, California. Prior to that, she worked at Philadelphia Eye Associates and was affiliated with Wills Eye Hospital and the University of Pennsylvania’s Scheie Eye Institute, where she completed her glaucoma fellowship and ophthalmology residency.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

