Survey: America’s Bad Eye Care Habits
Home /
Most people are aware they need to look after their physical health, we’re often told to eat healthier and exercise more. But many of us neglect one key part of our body’s wellbeing: our eye health.
Table of Contents
With the pandemic affecting our lives, booking an eye exam or looking after our eyes may not have been our top priority. One study from August 2021, shows that there has been a sharp rise in near-sightedness among children due to increased screen time during this period.
To find out more about our current eye health habits, we spoke to over 1,200 Americans to ask how people care for their eyes and what potential downsides there could be to such choices.
Key Findings
- 1 in 10 (9.8%) have not had an eye exam in over 5 years, with 23% saying the pandemic is to blame for not having a recent (<1 year) appointment
- 2 in 3 (66%) leave daily disposable contact lenses in overnight and re-use for multiple days
- 25% wash contact lenses incorrectly opening up bacterial risk
- 1 in 4 (25.4%) wash their glasses once a month, or even less than that
- 83.6% ignore 20-20-20 rule recommended by American Optometric Association causing eye strain
- Almost half 48.9% not using blue light filters on smartphones
- 73% using air conditioning or fans at night, leading to dry irritated eyes
- Bad Habits: Eye Exams
Bad Habits: Eye Exams
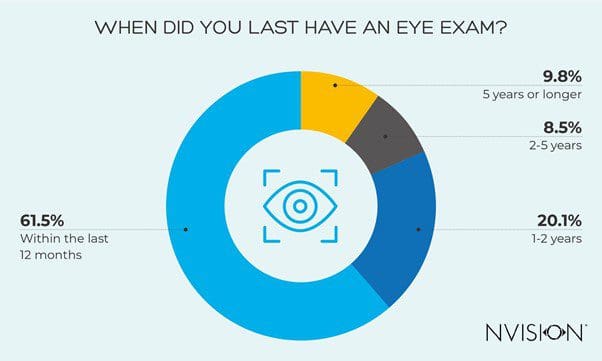
Getting your eye health check ups at least once a year is important to make sure your needs have not changed, and that your eyes are still in good shape. Our survey found that 38.5% of people have not had an eye exam in the last year.
Almost 1 in 10 (9.8%) have not had an eye exam in over 5 years
Breaking the data down further, we found that 9.8% said they hadn’t had an eye exam in over 5 years. Generally, 6 in 10 (61.6%) stated they had had an eye test in the last 12 months, with a further 20.1% in the last two years.
Understandably many people may not have been able to access eye exams due to the pandemic and we wanted to look at the impact this may have had on the nation’s eye health.
COVID-19 caused 1 in 5 (23.1%) to miss an eye exam
When asked if they had missed their eye exam due to the pandemic, and not yet rebooked, 23.1% stated that they were in this position. 25.9% said they had previously missed their appointment due to COVID but had since attended in the last 12 months.
Dr. Franklin Lusby, board-certified ophthalmologist, here at NVISION, who has performed over 70,000 refractive procedures, had this to say on people missing eye exams:
“There are a whole host of eye problems that have no symptoms. Although these types of problems are more likely to occur in older individuals, a significant number can be found in younger people. Many of these can only be discovered during an actual physical eye exam. Even though the pandemic has emphasized the value of tele-medicine, we have to recognize that it has its limitations. Working from home will have undoubtedly exacerbated this need for eye exams.”
“A big challenge is to identify the problem that has no symptoms because, with many of these, if left undiagnosed, damage can occur that may not be recoverable. Glaucoma is a relatively common condition that falls into this category. However, in an otherwise healthy, young population, it’s probably a minority of routine eye exams in which a problem will be uncovered that has no symptoms.”
Over 16 million people driving vehicles with untested vision
2020 figures from the US Census Bureau state there are around 231.652 million registered drivers in America, and it’s estimated that 30% of the population needs corrective eyewear to drive. This would mean around 69,495,600 drivers currently require eyewear to drive.
With approximately 23.1% missing their eye exams due to the pandemic, this could mean over 16 million (16,053,483) are driving with untested eyes where prescriptions may have changed, or other vision problems may have occurred since March 2020.
Bad Habits: Contact Lenses
Part of our survey was dedicated to asking our sample how they use contact lenses (if they use them) and whether they have any bad habits associated with them. Turns out, they do.
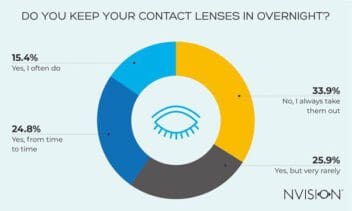
2 in 3 are leaving daily contact lenses in overnight
Put simply, daily contact lenses are absolutely not designed to be worn for more than one day, this does not include nighttime. Of those who use daily lenses, just over a third (33.9%) said they ‘always’ take them out. The rest of the respondents (66.1%) admitted to leaving them in overnight, with 15.4% saying this happened ‘often’.
Dr. Max Parikh, board-certified, and award-winning ophthalmologist at NVISION, had this to say on why you should not leave contact lenses in overnight:
“Contact lenses are foreign bodies made of soft or hard plastic and it is not natural for them to remain on your eyes for long periods of time. Thus, redness, irritation, and pain are common with even routine contact lens wear. When worn overnight, eyelids are closed, and less oxygen and tear film circulation occur around and under the contact lens. This also becomes an ideal environment for bacteria, fungus, and parasites to accumulate. These microorganisms can then cause infections on your cornea by either entering through micro abrasions or even intact surfaces.”
“There is a 6-8 times higher risk of infection when contacts are worn overnight vs during day hours only. 11-13% of such infections result in permanent vision loss despite medical and surgical treatments.”
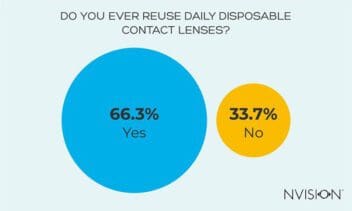
2 in 3 admit to reusing daily contact lenses
The risks of reusing daily contact lenses include a host of bad things: infections, dryness, visual impairment, and even corneal scarring. In short, it’s not good for our eye health to use them past their intended one-day usage.
Of our sample, 66.3% admitted that they do reuse daily contact lenses, which is not far from results published by the American Optometric Association (AOA). Their study found that almost half of contact lens wearers (including daily lenses) were wearing them for longer than the recommended time.
Dr. Franklin Lusby, board-certified ophthalmologist, at NVISION, discussed the dangers of reusing daily contact lenses.
“Daily disposable lenses are associated with the lowest infection rates since the lenses should never be slept in, and a new pair should be inserted each day so that there is no chance that you are putting a contaminated lens in your eye. But these lenses are usually very thin so that, although they may be good for transmitting oxygen, over time, they tend to lose their shape characteristics and they don’t hold up to disinfecting routines very well.”
“The advent of daily disposable lenses has eliminated a whole host of problems; each day you have brand new lenses so optical parameters and potential contamination fly out the window. Further, for people who make protein deposits, it has been a godsend. However, the infection risk of re-using a daily disposable lens is in a worse category than the proper use of any daily wear, reusable lens. One study out of Hong Kong found a 45% contamination rate with Staphylococcus in daily disposable lenses after one day of re-use; clearly not worth the risk.”
Aside from daily lenses, we also wanted to find out how contact lens wearers were cleaning their lenses between uses.
1 in 4 are putting their vision at risk by not cleaning contact lenses correctly
Dr. Franklin Lusby, board-certified ophthalmologist, comments on cleaning contact lenses:
“Tap water should have no place in a contact lens care regimen. One of the most serious corneal infections is acanthamoeba keratitis. It was discovered in the 1980s in contact lens wearers. Two prevalent risk factors identified in those studies were 1) use of tap water to make homemade contact lens solutions and 2) swimming in a pool or hot tub while wearing contacts.”
“Many cleaning solutions today are multi-purpose: cleaning, rinsing, disinfecting, and storage. Most commercially available solutions today can be used with most soft contact lenses. However, certain lens types (such as rigid gas permeable) may require special solutions and care; for that, you will need to follow your eye care professional’s advice.”
Despite this being the industry professional advice, 18.3% of respondents said they use tap water to clean their lenses, while 7.1% said they don’t actively wash them.
Thankfully, the majority (74.5%) are using a bottled contact lens solution to clean their lenses. If you use anything other than contact lens cleaning solution, you could be exposing your eyes to a whole host of eye health complications.

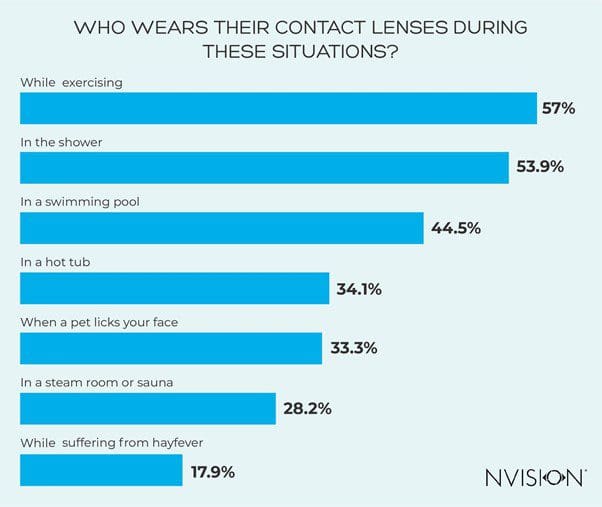
2 in 5 are wearing contact lenses when swimming
Swimming when wearing contact lenses can be problematic due to the simple fact that water is likely going to get into your eyes, and on your contact lenses. Over 2 in 5 (44.5%) revealed to us that they leave their contact lenses in for swimming.
Dr. Lusby, board-certified ophthalmologist, comments on swimming with contact lenses, and whether goggles may be a safe option:
“Theoretically, if not a single drop of water gets in your eyes, then wearing tight-fitting goggles over contact lenses would be ok, but, as a lap swimmer (who doesn’t wear contacts) I can tell you: that is virtually impossible, especially as you are removing your goggles. Plus, the goggles that never leak don’t exist. Furthermore, excessively tight goggles can be a bad idea for other reasons.”
“The problem is that pool water can carry with it contaminants that can potentially cause an infection. But more than that, the chlorine may disrupt the corneal surface a bit and make you more susceptible to infections.”
We also asked our respondents about a range of situations where wearing contact lenses can lead to potential eye health problems. Exercising can be dangerous due to lenses moving around or getting knocked out, however this is often a preferable choice compared to glasses.
Showering can cause tap water’s bacteria to infect your lenses, and a hot tub is dangerous in similar ways to a swimming pool. Contact lenses should be avoided when in a sauna as they can cause your lenses to dry out, but the moisture in the air can also present bacterial problems too. Such germs and bacteria can also be present when pets are showing affection by licking your face, if you have contacts in, it can be a dangerous situation.
Finally, hay fever can cause pollen to get trapped under your contact lenses if you rub them, Dr. Lusby, continues, commenting on the best way to wear contact lenses when suffering from hay fever and other allergies:
“In one recent study, 75% of people with allergic rhinitis (hay fever) also had allergic conjunctivitis. The release of histamines that occurs in an allergic reaction is responsible for the swelling of the tissues around the eye, and the redness and itching; this may be a somewhat inhospitable environment for contact lens usage. Symptomatology often parallels pollen counts, especially during seasonal episodes.”
“If you are able to wear your contacts during a bout of hayfever, there is no particular negative effect that will occur. If you need to instill eyedrops, unless they are lubricating drops designed to be used with contacts, you should remove your contacts, instill the drops and then wait about a half hour before re-inserting your contacts. This allows the active agent in the eyedrop to be absorbed without interference from the presence of a contact lens and will help prevent things like preservatives from accumulating and concentrating in the contact lens.”
“If you choose to continue your contacts through a bout of allergy, it is usually a good idea to increase the use of an approved-for-contacts lubricating drop even though your eyes may be running and wet.”
Bad Habits: Glasses
While glasses don’t carry all the same risks as contact lenses, as they aren’t being placed directly onto your eye, they do still need to be cleaned. One 2018 study found they can grow the bacteria that causes staph infections, and they can also lead to poor skin health causing blackheads and acne. In short, glasses wearers need to be cleaning their frames at least once a week, and their lenses daily.
1 in 4 wash their glasses once a month or less
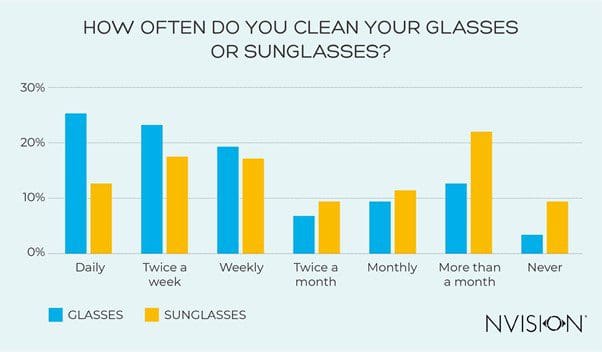
Far from the weekly recommendation, almost a quarter (25.4%) stated they wash their glasses once a month, or even less than that. The majority (67.7%) are washing their glasses at least once a week, with a quarter (25.1%) of this group ensuring this happens on a daily basis.

For the same hygiene reasons, sunglasses also need to be cleaned daily, especially during the summer months when we are more likely to wear them every day.
Over half (52.5%) clean their sunglasses twice a month or less
Generally, we’re better at cleaning our glasses than we are our sunglasses. A quarter (25.1%) said they clean their glasses daily, but only 12.9% would clean their sunglasses daily (in a period where they would be worn regularly).
Dr. Lusby, board-certified ophthalmologist, comments on cleaning your eyewear:
“Most professionals recommend cleaning your glasses every day or two, but that would also depend on what your skin is like, how much makeup you wear, etc. Since much of the debris that collects on eyeglasses is mixed with oil (from the skin) using dish soap to clean is not a bad idea. But if you want to go a step further, using an ultrasonic cleaner (home units are usually sold as jewelry cleaners) with the recommended solution would be the ultimate option.”
“It’s never a good idea to clean or dry your glasses with a paper towel or similar product; there’s too much potential for scratching the lenses.”
Bad Habits: Screens & Electronics
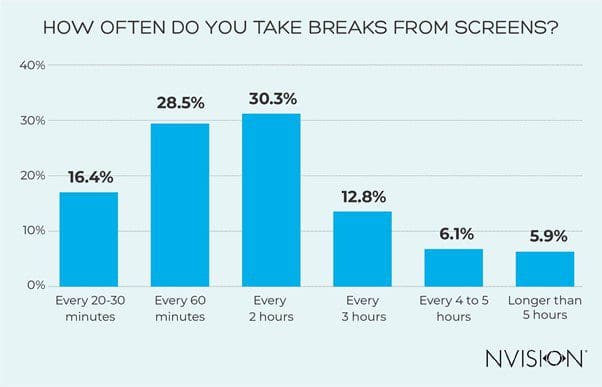
We all know too much screen time is bad for us, and our eye health experts will always recommend using the 20-20-20 rule. In short, it encourages you to spend 20 seconds looking at something 20 feet away for every 20 minutes of screen time. Our survey found that only 16.4% of regular screen users were taking screen breaks at this recommended interval.
83.6% are ignoring the 20-20-20 rule from the American Optometric Association, creating eye strain environment
The most common break period for regular screen users was every 2 hours (30.3%), way beyond the recommended 20 minutes.
Dr. Lusby, board-certified ophthalmologist, comments on screens and eye health:
“Fortunately, most symptoms from excessive screen time are reversible and not associated with permanent damage. The most common issue would be dryness since studies have shown that blink rate during screen time is about half of what it is ordinarily. If there is poor contrast or poor resolution, this can lead to mental fatigue due to the increased amount of image processing required”
“Numerous studies have shown that, over the decades, as our society has become more of an “indoor” society, the overall prevalence in the population of myopia has increased. Although some have suggested that the prevalent wavelengths of outdoor light are a factor in this, it more likely has to do with what the eyes are focused on: a distant object or a near object. This would suggest that it’s the screentime on a smartphone or tablet that may be a significant culprit since a laptop or desktop screen is likely viewed at a further distance. The impact of these behaviors is real; as a refractive surgeon, I have no shortage of patients who will tell me that they didn’t get nearsighted until after college or grad school (far later than what one would expect based on the standard demographics of myopia) and they attribute it to all of the reading and computer use.”
“During the pandemic, virtually anyone who works or goes to school has seen an explosive increase in their screen time. It’s become a way of life and, for most people, there’s no real way around it. Whatever eye fatigue problems in this regard that may have existed prior to the pandemic, have only been magnified. Taking the proper breaks and having the proper habits are more important now than ever.”
Only half (52.9%) turn their phone brightness down before bed
Taking breaks from screens is one way to help your eye health when using devices, another is to control the brightness settings, especially when in a dark environment, like before bed.
Overall, 52.9% said they actively turn the brightness down before bed, with 34.7% saying they leave it on their daytime setting, and a further 12.4% preferring to turn the brightness up as they’re in a dark environment.
Dr. Lusby, board-certified ophthalmologist, comments on optimal screen conditions:
“There are two main parameters for screen adjustment: contrast and brightness. Brightness is best determined by the ambient light in the environment. Higher ambient light will require higher brightness. Contrast will also come into play; it may be possible to get by on less brightness by increasing the contrast. The goal is to adjust these so that the mental energy you have to expend in image processing is minimal.”
“Brightness and/or contrast that are too low can lead to eye strain and mental fatigue but both of these problems should be temporary.”
Half (49%) not using blue light filters on smartphones
We also asked our respondents about blue light filters and whether they use them on their phones. Studies suggest that too much blue light can impact our sleep and possibly damage our retinas, but it’s important to note that studies are still small and inconclusive.
With the potential dangers of blue light in mind however, it’s interesting to see that there’s almost a half-half split on whether phone users are using such features.

Of those who do use a blue light filter, 31% said that they use it regularly, or all the time, indicating that they turn it on outside of the default settings (after sunset).
Dr. Lusby, board-certified ophthalmologist, comments on blue light:
“Too much blue light can impact our sleep habits, metabolism, and visual acuity (the clarity of your vision). One study suggests that blue light could speed up macular degeneration, which is the most common cause of blindness. There are many myths out there about how truly dangerous it is, and importantly, studies simply don’t have all the answers yet.”
“It should be said that blue light can be good for you as it makes you feel more awake and alert, and can be beneficial on memory and mood. Additionally, most authorities agree that blue light, at the normally encountered levels one would typically find, causes no permanent damage to the eye”
Bad Habits: Hot Nights
Finally, we asked our respondents about air conditioning and fans, crucial to our comfort in hot weather, but a potential irritant to our eyes when sleeping.

Aircon causes us to have dry eyes so having them on all night can be bad for our eye health causing redness, itching, or even blurred vision. Additionally, fans can have a similar effect, but they can also be responsible for blowing in eye irritants like dirt and pollen from outside, especially if placed next to a window. Therefore, if you have the fan pointed at you while you sleep you may be causing your eyes to get red and irritated further.
Methodology
The survey was conducted via Amazon’s Mechanical Turk platform collecting responses from 1,209 Americans from a range of backgrounds from 26th July – 8th August 2021. The demographic breakdown of our respondents is as follows:
Gender:
- Female (59.22%)
- Male (40.2%)
- Other (0.58%)
Age:
- 18-24 (11.66%)
- 25-35 (39.95%)
- 35-44 (23.74%)
- 45-54 (12.57%)
- 55-65 (8.44%)
- 65+ (3.64%)
References
- Myopia incidence and lifestyle changes among school children during the COVID-19 pandemic: a population-based prospective study (August 2021). British Medical Journals: British Journal of Ophthalmology
- Myopia (nearsightedness) American Optometric Association
- Contact Lens Care American Optometric Association
- Ambient bacterial load of frames and lenses of spectacles and evaluation of different cleaning methods (November 2018). PLos One
- The Best Ways to Clean Your Eyeglasses (November 2018). Healthline
- Blue light excited retinal intercepts cellular signaling (July 2018). Scientific Reports
