
Medically Reviewed by Angelique J. Pillar, M.D. NVISION Surgeon
What Is Corneal Cross Linking? (Pros and Cons in 2024)
Home / Laser Eye Surgery Guide (Updated) /
Last Updated:

Medically Reviewed by Angelique J. Pillar, M.D. NVISION Surgeon
When the collagen tissue in the front part of your eye weakens, the cornea bulges to form a cone-shaped structure instead of the usual round shape. Such a warped cornea causes keratoconus with blurry vision. Corneal cross-linking surgery prevents progression of the corneal damage by strengthening the fibers in your eye, stabilizing your vision.
Table of Contents
While the condition of keratoconus is primarily hereditary, it can develop in the wake of eye surgeries such as LASIK. With riboflavin, vitamin B2 (as a photosensitizer), an ophthalmologist will use ultra-violet light to strengthen the bonds connecting collagen fibers in your affected eye to alleviate or resolve the symptoms of keratoconus.
This is a relatively new procedure, as it was only approved by the U.S. Food and Drug Administration in 2016. Even now, only one method of the surgery is approved, and it’s a solution that is made just for people with stable keratoconus.
The surgery can be very helpful, but the approved method involves removing part of the eye, and recovery is painful. Doctors are testing a different approach that keeps eye structures in place, but it has not been approved yet.
If you choose to move ahead, the research suggests the procedure can stop the progression of keratoconus, and your vision might even improve. Your insurance company might pay for the care you need.
What Happens During Cross-Linking?
Keratoconus causes your eyes to take on a pointed, rather than a round, shape. Doctors think that weakness and poor connections are to blame. When the tissues in your eyes are loosely attached to one another, they can drift apart and harden in new configurations. Without treatment, the problem gets worse.
Cross-linking is a simple procedure that is performed in the outpatient department as a day case. You will therefore return home the same day, not long after the surgery. Here is what to expect during the operation:
- Anesthetization: As you lie down, the doctor will give you medications to relax and administer eye drops to numb your eyes. You will therefore not feel any pain throughout the procedure.
- Abrasion of corneal epithelium: the doctor scrapes off the outer layer of your cornea to allow penetration of medication to the inner corneal tissues.
- Vitamin B2 application: A special solution of vitamin B2, which acts as a photosensitizer, is applied to the cornea every three minutes for half an hour.
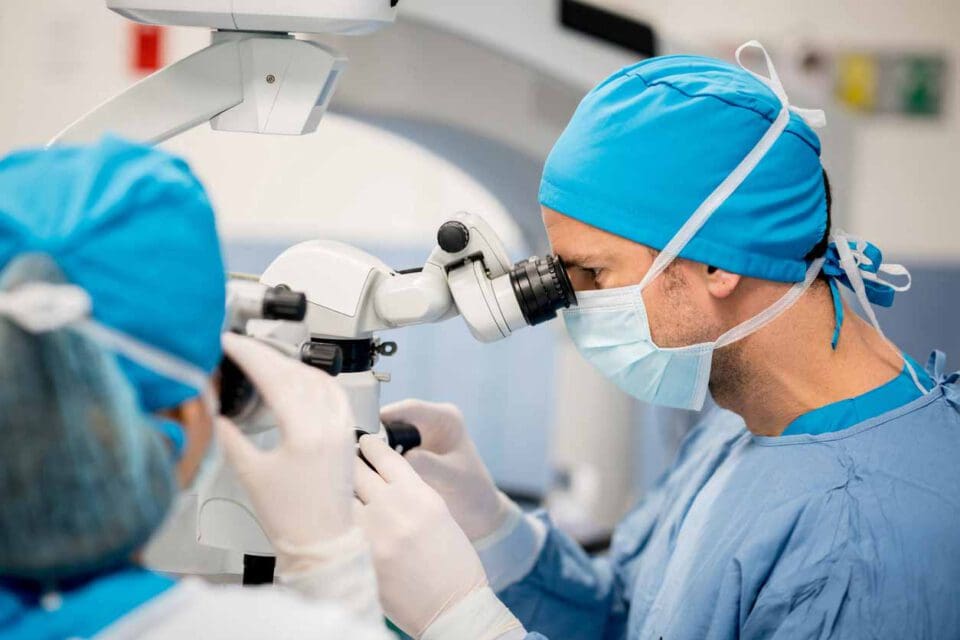
- Corneal irradiation: using an optical system, the doctor focuses a beam of UV light on your cornea for about 30 minutes. The light rays activate the vitamins in the eye leading to the formation of new connections between the collagen fibers in your eye.
- Bandaging: to promote healing, the doctor applies a contact lens bandage to your eye, which should remain in place for about seven days.
Who Does Cross-Linking Help?
This surgery is designed for people with keratoconus, and it’s appropriate for those who were born with the problem and those who developed it after surgery. But it’s not the right solution for every person.
If you have keratoconus that developed after surgery, cross-linking should help to amend the damage and heal the shape of your eye.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
If you have the hereditary form of the disease, the answer is a little more complicated.
Hereditary keratoconus is progressive, and it does tend to get worse early in young people. But when you move into adulthood, you may have a “stable” form of the disease. Your eyes may not get better, but the shape of your corneas will not change each year.
Researchers say cross-linking is approved only for progressive keratoconus. If your eye has stopped changing each year, the surgery is not recommended for you.
The American Academy of Ophthalmology reports that the surgery is not right for people with:
- Thin corneas. A thickness of 400 microns or more is required.
- Infections. Current infections or a prior herpes diagnosis leave your eyes at risk.
- Scars. If your corneas bear the marks of previous injuries, you might be at risk for complications.
- Dry eyes. Your eyes need tears during recovery. If you struggle to produce that substance, you might not heal nicely.
- Autoimmune disease. This can up your risk of poor wound healing.
Should You Wait to Have Surgery?
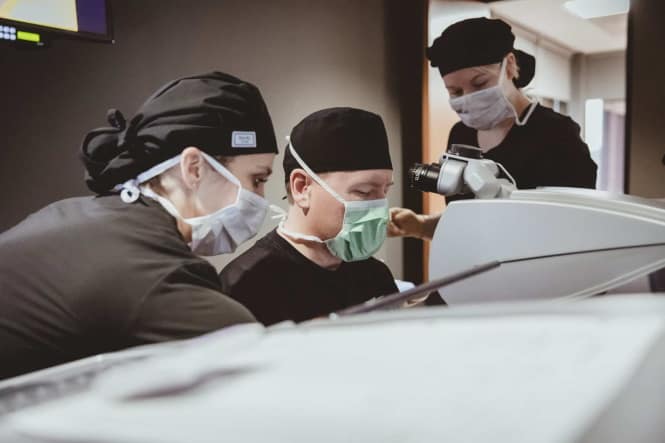
If you are approved for a surgical correction, should you set it up right away? This is a relatively new procedure, and there are some things researchers do not know quite yet. Also, only one form of the surgery is approved, and it might not be right for you. But waiting comes with risks too.
Types of Keratoconus Surgeries
The treatment of keratoconus can involve either the removal of the corneal epithelium (epi-off) or retention of the epithelium (epi-on). Surgeons debate the merits of one procedure over the other, with some arguing that epi-on gives a faster recovery and less pain while others suggest epi-off is superior with a better surgical response.
At the moment, epi-off stands as the only method approved by the FDA for keratoconus treatment.
EPI-Off
In epi-off, up to 7 mm of the corneal epithelium is removed and vitamin B2 solution is applied to the cornea after every 3 minutes for half an hour. Ultra-violet light is then used to radiate the riboflavin-saturated cornea leading to the formation of stronger interfibrillar and intrafibrillar bonds thereby preventing keratoconus progression.
EPI-On
For the epi-on technique, the epithelium is left intact but different substances are used to loosen the epithelial tight junctions and promote penetration of the vitamin solution. Compared to the epi-off, this method limits the uptake of riboflavin, which leads to less satisfactory surgical outcomes. If you have stabilized keratectasia, epi-on can be more beneficial with lesser pain and faster recovery.
Will Your Insurance Pay?
Blue Cross Blue Shield of North Carolina says, for example, that the treatment can be considered a covered benefit for people who tried conservative keratoconus therapies and still got worse. If you haven’t tried reshaping contact lenses or other routine treatments for eye shape, your doctor may require you to take those steps before scheduling surgery if you hope to use your insurance benefits.
Blue Cross Blue Shield of Tennessee says that this is a covered benefit only if your surgeon uses the epi-off method. If your doctor leaves the epithelium in place, the insurance company considers this an experiment, and no payment will be given.
Since insurance rules can be hard to understand, it’s best to ask your doctor to check your coverage before your surgery. That way, you will know how much you will have to pay after insurance. You can also find out if your coverage does not extend to corneal cross-linking, so you will not set up a surgery you can’t pay for.

You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Does Cross-Linking Help?
Before you check benefits and make surgical plans, it’s best to ensure that the surgery has a reasonable chance of helping you to feel better. Current research suggests that this is an exceptional solution for people with keratoconus.
In one study published in 2017, researchers split people into two groups. One set had keratoconus and got no treatment. The other got epi-off cross-linking. At the end of the study, 86.7 percent of people had improved keratoconus after surgery, while only 26.7 percent of people with no surgery got better.
It’s important to note that surgeons don’t promise that you will have better vision after surgery. Instead, they tell you that your eyes will not continue to change shape. Even so, some studies suggest that people really do see better after cross-linking.
In a 2014 study, researchers found that about half of people who had cross-linking had an improvement of one line in visual acuity two years after surgery. These people probably still needed glasses, but their prescriptions were smaller.
Studies like this demonstrate just how powerful this treatment can be for people with keratoconus.
What to Know About Recovery

While reading up on results is exciting, particularly for people with difficult eye problems lasting for years, this is a major eye surgery. As a result, the recovery can stretch on for weeks or even months.
You will head home from surgery with eye protection. The next day, your eyes might feel:
- Hot
- Gritty
- Dry
- Painful
You will have eyedrops and pain medication to use when the discomfort grows severe. You will also notice shifting vision.
Experts say your vision can change during:
- Months one to three. Each day, your acuity might be a little different.
- Months three onward. Your vision may stabilize, but you may still see fluctuations. The curve of your eye may change during this time.
You will not have contact lenses to ease your shifting vision, as your eyes will need oxygen to heal. Your glasses may not help either, as you might need a new prescription for each day or even each hour.
Stay calm, and work with your doctor. It’s helpful to hear that these issues are both natural and expected, and your doctor may have tips that can help you to get through the healing process with your sanity intact.
You can speed healing by:
- Using your eye drops. Lubricated eyes heal faster and are less gritty.
- Keeping your hands to yourself. Rubbing your eyes causes damage.
- Using sun protection. Bright sunlight makes you squint, and that can hurt your healing eyes.
- Sleep. Tissue repair is a key part of sleep. Make rest a priority.
If you think your eyes are not healing properly or you have any other concerns, talk with your doctor right away.
When your eyes have healed and your vision has stabilized, you can work with your doctor on a new eyeglass prescription. You will know that your glasses will not be out of date in a few weeks due to eye shape, and that could be a big relief to you. But you will need to take care of your eyes as they heal.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Benefits of Cross-Linking Go Beyond Stopping Progression of Keratoconus. (January 2016). Ocular Surgery News.
- Corneal Collagen Cross-Linking. (January 2016). American Academy of Ophthalmology.
- Corneal Cross-Linking: Current USA Status. Report from the Cornea Society. (October 2018). Cornea.
- FDA Approves First Corneal Cross-Linking System for Treatment. (July 2016). American Optometric Association.
- Epi-Off Versus Epi-On Corneal Collagen Cross-Linking in Keratoconus Patients: A Comparative Study Through 2-Year Follow-Up. (2018). Journal of Ophthalmology.
- Corporate Medical Policy: Corneal Collagen Cross-Linking. BlueCross BlueShield of North Carolina.
- BlueCross BlueShield of Tennessee Medical Policy Manual: Corneal Collagen Cross-Linking. (June 2018). BlueCross BlueShield of Tennessee.
- Determining the Efficacy of Corneal Crosslinking in Progressive Keratoconus. (March 2017). Pakistan Journal of Medical Sciences.
- Everything You Need to Know About Corneal Collagen Cross-Linking. (May 2016). New Grad Optometry.
- Analysis of 2-Year Corneal Cross-Linking Results in Keratoconus Patients. (2014). Journal of the Egyptian Ophthalmological Society.
- Corneal Collagen Cross-Linking. (March 2010). Middle East African Journal of Ophthalmology. Date fetched: August 7, 2021.
- FDA approves first corneal cross-linking system for treatment. (July 12, 2016). American Optometric Association. Date fetched: August 7, 2021.

Angelique Pillar, MD, is a cataract, cornea, and refractive surgeon with over a decade of post-fellowship experience and a proven track record of excellent surgical outcomes.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

