
Medically Reviewed by Angelique J. Pillar, M.D. NVISION Surgeon
Corneal Transplant Surgery: Costs, Success Rates & More
Last Updated:

Medically Reviewed by Angelique J. Pillar, M.D. NVISION Surgeon
Several factors can cause irreversible damage to the cornea, from eye infection to trauma. For some patients who can’t see well because of this problem, corneal transplant (Keratoplasty) is the only viable option to restore their vision.
Table of Contents
This eye surgery gives tens of thousands of patients hope for clear vision each year. In 2019, U.S. doctors performed 66,278 corneal transplant procedures.

The nature or severity of the damage will determine what other remedies may be worth exploring besides eye surgery. Also, a thorough examination will reveal the specific parts of the cornea that require replacement.
After identifying any damaged tissues, your ophthalmologist can select an appropriate type of keratoplasty. Many of these procedures have a high success rate.
If you’re nervous about having corneal transplant surgery, knowing what to expect of the procedure can ease some of your concerns.
Who Needs a Corneal Transplant?
Corneal transplant surgery is one of the treatment options your ophthalmologist may recommend if you have severe corneal damage. It’s generally a last-resort measure when remedies like prescription eyewear can’t improve or restore your eyesight.
Although contact lenses work for many patients with a damaged cornea, wearing then may be impossible, or else they can cause side effects. For patients with lens intolerance, surgical replacement of the scarred or diseased corneal tissue may be necessary to correct visual defects.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Some of the vision problems that a cornea transplant can treat:
- When keratoconus is the cause of your corneal damage: With this medical condition, the cornea bulges outward, steepens, and becomes too thin, forming a cone shape. According to the National Keratoconus Foundation (NKCF), eye doctors recommend transplant surgery to 15-20% of patients with this condition.
- Fuchs’ dystrophy: This disease occurs when the corneal inner layer malfunctions, causing fluid to build up inside the cornea. You’re unable to see clearly as the cornea swells and becomes cloudy.
- Eye Infections: A bacterial attack can cause swelling and irreparable damage to any part of the cornea. If treating the infection doesn’t heal or repair the affected corneal layers, surgical tissue replacement may be the only practical remedy.
- Corneal injury: Abrasions on the surface of the cornea or the physical tearing of deeper corneal layers can also cause severe vision problems.
- Eye surgery: This is accidental injury to the cornea during previous surgery on the cornea or any other part of the eye.
What Does a Corneal Transplant Do?
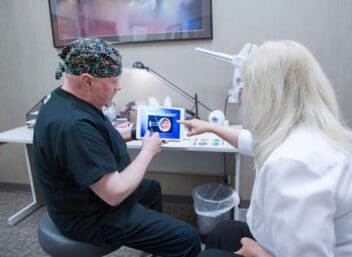
A corneal transplant can restore vision by having a healthy cornea replace a damaged corneal through microsurgery. The new cornea comes from a human donor. Eye tissues are tested for quality and safety before transplantation.
Careful screening helps improve the chances of treatment success and minimizes the risk of post-surgery complications.
If you have extensive corneal damage, the entire cornea will be removed and replaced with a clear, healthy one. Otherwise, only the scarred part of the cornea requires transplantation.
Once a smooth and healthy donor cornea is in place, your vision should start improving.
What to Expect: Things to Do, Avoid and Expect Before Surgery
You may need to make certain changes in your everyday routine to be better prepared for a corneal transplant. Your doctor likely will recommend a list of habits or behaviors to change, to avoid and to do in the runup to surgery.
- Discuss Concerns: If you have any concerns over the procedure, discuss those with your ophthalmologist weeks before the surgery day. You can talk about possible treatment outcomes and risks (and how these might affect your everyday living in the short and long term).
- Review Your Current Medicines: Discuss any medication or supplements you currently take. If you’re taking blood thinners, even something minor such as aspirin, you should let your ophthalmologist know. (This goes for any surgical procedure.) Aspirin and blood thinners prevent clotting, and having them in your system during surgery can cause excessive bleeding. If you must take prescription drugs that could complicate your transplant treatment, your doctor may recommend delaying the procedure until you finish your current dose or regimen.
- Mind Your Physical Health: Successful treatment and recovery can depend largely on the state of your health at the time of surgery. Don’t assume that issues like infections or inflammation will go away without treatment or have no effect on your corneal transplant. To ensure you’re physically fit for the scheduled operation, let your doctor run some tests. You may need to use certain medications to treat any worrisome complications discovered before surgery.
- Arrange for Transport Home: It’s never safe to drive yourself home right from the operating room. You wouldn’t be in an ideal frame of mind for this because of any medication or even anesthesia left in your system. Since corneal transplantation is an outpatient procedure, you can have someone drive you to the hospital and back home.
- Wait on a Healthy Cornea Donation: Once you feel confident about having a corneal transplant, let your ophthalmologist know right away. It shouldn’t take long to find a good donor cornea in a local eye bank. The surgeon can then schedule your surgery and inform you accordingly.
What to Expect the Day of Transplant Surgery

Here’s what happens when you enter the operating room:
Pain Management
Your ophthalmologist may give you calming medication before surgery. Sedatives will help you relax, especially if you prefer to stay awake during the procedure.
General anesthesia may be administered to put you to sleep. If a local numbing agent is used instead, you’ll be awake but won’t feel any pain throughout the procedure.
Surgery
Your surgeon will use a special instrument to keep your eyelids open and expose the site of surgery. The exact next steps depend on the type of corneal transplant surgery needed to restore your vision.
Generally, only the scarred or diseased part of the eye is removed and replaced with a healthy equivalent from a donor. Your surgeon may cut out the following damaged eye parts/tissues:
- Your entire cornea
- Layer of cells from the surface of the cornea
- The middle section of the cornea
- The innermost layer of the cornea
For any section of the cornea removed, a healthy match from a donor is sewn into place. However, the procedure for replacing the inner layer differs slightly from the others.
Instead of stitching, your surgeon will use an air bubble to neatly secure the deeper corneal tissue into place.
The fresh site of surgery remains vulnerable to infection and injury for a brief period before healing. For this reason, a protective shield will be placed over your eye after the outpatient procedure.
It’s important that you adopt the right self-care practices after surgery to get the best possible outcome. You can discuss these measures with your ophthalmologist before going home.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Post-Operative Care and Recovery
Here’s what to keep in mind to prepare for successful recovery after your corneal transplant:
- Your repaired corneal tissue is extremely delicate during the first 24 hours following surgery. This wouldn’t be an appropriate time to resume your daily routine.
- The lack of immediate vision improvement doesn’t necessarily mean that your corneal transplant is failing. It can take a year or longer before your cornea heals and functions as intended.
- You’d typically have a follow-up eye checkup the day after surgery. If there are any early issues, your eye surgeon can spot them and recommend appropriate treatment right away.
- Your ophthalmologist may recommend briefly lying on your back when you go home after surgery. With your face up, you can avoid disturbances that may dislodge the new corneal tissue out of position.
- Your ophthalmologist will decide when to remove the stitches from surgery. Your pace of recovery, as observed during routine eye exams, will determine this.
- You should protect your eyes from physical trauma or any type of external pressure. Wearing eyeglasses or an eye shield is highly recommended.
- Don’t rub your eye, even if it’s itchy.
- You’ll need to use prescription eye drops to control any infection or swelling in the eye.
- If you experience any soreness in the eye after surgery, you can use over-the-counter painkillers.
Risks and Success Rates
Most patients with a damaged cornea notice restored vision with corneal transplant surgery. They can enjoy these benefits without any complications for at least 10 years, according to the National Health Service.
Treatment success depends on the type of corneal transplant you had. If you had your entire cornea replaced, you might experience complications not common with other types of corneal transplants.
Risks With Corneal Transplant
Some patients experience cornea rejection and other eye disorders following transplant. About 70% of patients experience no rejection.
Cornea rejection

In 3 out of 10 patients who have their entire cornea replaced (full thickness transplant), the body fights and rejects the new tissue. Other types of corneal transplant have a lower rejection rate.
Medication can correct this problem, and if it doesn’t work, the patient may require another corneal transplant.
Common signs of cornea rejection after surgery include:
- Persistent eye pain
- Abnormal sensitivity to light
- Blurry vision
- Red eyes
Eye Disorders
A number of post-surgical disorders can come in the wake of surgery. Among them:
- Glaucoma: Keeping your eye pressure within a normal range can prevent damage to your optic nerve.
- Uneven cornea or astigmatism: To fix this vision problem, your ophthalmologist may loosen or tighten some of the stitches securing your new cornea in place.
- Infection: Using prescription eye drops and any other antibiotics your ophthalmologist prescribed should help prevent or control any bacterial infection in your eye.
- Retinal detachment: With this condition, the retina (at the back of the eye) separates from the tissue that sustains it. It’s usually a medical emergency because it can cause vision loss.
See your ophthalmologist if you experience any unusual vision issues after surgery. Also, don’t miss your follow-up appointments, including a year or longer after the procedure.
During these regular post-surgery checkups, your eye doctor can spot any early signs of post-surgery complications, some of which can occur long after treatment.
Corneal Transplant Costs
How much corneal transplant costs depends on variable factors, including your age and the type of surgery you had. Your post-operative care will cost more if you experience major emergencies.
On average, a full-thickness corneal transplant costs $18,900 for a patient younger than 65 and $16,700 for those who are 65 or older. These estimates are for the following outpatient medical services:

- Anesthesia
- Ophthalmologist
- Facility, including cost of the corneal tissue
- Services before surgery, including physician consultation and lab exams
- Post-surgery care, including follow-up consultations, drugs, checkups, and vision correction
- Medication, including antibiotic and steroid eye drops
If you have a personal health plan, such as Medicare, insurance will cover most of the corneal transplant costs. Your out-of-pocket expenses will usually include copays and coinsurance.
Different Types of Corneal Transplant Surgery (Keratoplasty)
Ophthalmologists use different surgical techniques to correct corneal damage. The right type of keratoplasty for you will depend on the part of the cornea to be removed and replaced.
This is usually determined during pre-operative eye tests. Here are the corneal transplant options you may be offered to treat your vision problem:
- When Your Entire Cornea Needs to be Replaced: Also known as penetrating keratoplasty (PK), full-thickness surgery is required when infection or injury causes irreparable damage to the front and inner layers of the cornea. Your surgeon will create small incisions on the eye to remove the damaged cell layers. New, healthy corneal tissue is then inserted through the incision and stitched into place. Since you’re getting an entirely new cornea, you may need a year or longer to recover and realize the full benefits of this treatment.
- When Only the Front and Middle Corneal Layers are Damaged: There’s no need to replace the entire cornea if only the front and middle layers are dysfunctional. In that case, your ophthalmologist will recommend deep anterior lamellar keratoplasty (DALK) to treat your eye condition. DALK is a partial-thickness transplant that can restore vision in patients with keratoconus. The operation replaces the outer and middle layers of the cornea. With this procedure, no incisions are made into the innermost layers of the cornea.
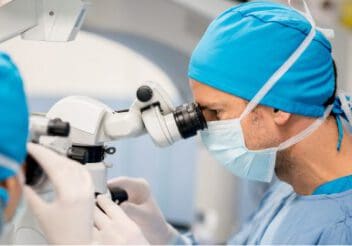
- When Only the Front Corneal Layers are Damaged: In some cases, only the outer layers of the cornea are replaced with healthy donor tissue. This procedure is called anterior lamellar keratoplasty (ALK). Since the surgical incisions don’t go deep into the cornea, ALK has a shorter recovery period than more intrusive techniques. Also, it has a lower risk of corneal tissue rejection.
- Replacing the Innermost Layer of the Cornea: Known as endothelial keratoplasty, this procedure focuses on the thin back layer of the cornea, leaving the front and middle layers intact. It has one of the fastest recovery times because there’s minimal interference with other parts of the cornea. Since only a small cut is made, many patients don’t require corneal stitches to keep the new tissue in place. Also, your body will more readily accept the healthy donor tissue after the transplant.There are two main techniques your ophthalmologist may use to transplant the innermost section of the cornea. These are:
- Descemet’s Stripping (Automated) Endothelial Keratoplasty (DSAEK): With this technique, your eye surgeon will replace the damaged inner section of the cornea with a healthy back layer from a donor. The transplant material for this procedure is thicker than in DMEK because it includes some corneal supporting tissue.
- Descemet’s Membrane Endothelial Keratoplasty (DMEK): With DMEK, your ophthalmologist replaces damaged inner layers with thin corneal tissue from a donor. In both DMEK and DSAEK, an air bubble is used to push the transplant into place.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Eye Banking Statistical Report. Eye Bank Association of America.
- Corneal Transplant. The National Keratoconus Foundation.
- About Corneal Transplantation. (September 13, 2021). American Academy of Ophthalmology.
- Cornea Transplant. (December 22, 2020). Mayo Clinic.
- Overview Cornea Transplant. (July 13, 2021). National Health Service.
- Cost-Benefit Analysis of Corneal Transplant. (September 2013). Eye Bank Association of America.

Angelique Pillar, MD, is a cataract, cornea, and refractive surgeon with over a decade of post-fellowship experience and a proven track record of excellent surgical outcomes.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

