
Medically Reviewed by Angelique J. Pillar, M.D. NVISION Surgeon
Corneal Dystrophy: Guide to the Types & Treatment
Home / Eye Conditions & Eye Diseases /
Last Updated:

Medically Reviewed by Angelique J. Pillar, M.D. NVISION Surgeon
Table of Contents
Corneal Dystrophy is a collective term referring to several conditions that cause a buildup of abnormal material in the corneal layer of the eye.
These disorders can lead to loss of vision and might necessitate a corneal transplant in severe cases. While some forms of Corneal Dystrophy develop in early childhood, others may not appear until middle age.

What Is Corneal Dystrophy?
Corneal Dystrophy encompasses a group of genetic eye disorders characterized by the abnormal accumulation of substances in the clear, outer layer of the eye called the cornea. These accumulations can cause a range of visual impairments and discomfort.
The dystrophies can be classified by their genetic cause, by the corneal layer affected, or by the material deposited. Common types include Fuchs’ dystrophy, keratoconus, and lattice dystrophy.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Most Corneal Dystrophies are inherited, non-inflammatory, and tend to affect both eyes. The progression of these conditions varies, and while some forms may cause significant vision impairment, others may have little to no effect on vision.
Types of Corneal Dystrophy
Corneal dystrophy comprises various types, each affecting different parts of the cornea and manifesting unique symptoms. Below is a comparison table, followed by a detailed explanation of each type:
| Type | Layer Affected | Typical Onset | Primary Symptoms | Treatment Options |
|---|---|---|---|---|
| Fuchs’ Endothelial Dystrophy | Endothelium | Adulthood | Blurred vision, discomfort | Eye drops, corneal transplant |
| Keratoconus | Stromal | Adolescence | Distorted vision | Contact lenses, surgery |
| Map-Dot-Fingerprint Dystrophy | Epithelium | Varies | Eye pain, glare sensitivity | Lubrication, surgery |
| Lattice Dystrophy | Stromal | Childhood | Clouding, lattice pattern | Laser therapy, surgery |
| Granular Dystrophy | Stromal | Childhood | Granular deposits, vision loss | Observation, surgery |
| Macular Dystrophy | Stromal | Childhood | Opacity, vision loss | Corneal transplant |
Fuchs’ Endothelial Dystrophy
Affects the endothelium layer of the cornea, leading to symptoms like blurred vision and discomfort. Treatment may include eye drops or corneal transplant.
Keratoconus
Begins during adolescence, affecting the stromal layer. Symptoms include progressive distortion of vision, with treatment ranging from specialized contact lenses to surgery.
Map-Dot-Fingerprint Dystrophy
This type affects the epithelium layer, causing symptoms like eye pain and glare sensitivity. Treatment typically involves lubrication or surgical removal of the affected epithelium.
Lattice Dystrophy
Characterized by clouding and opacity in the stromal layer, resembling a lattice pattern. Treatment may include laser therapy or surgical intervention.
Granular Dystrophy
Also affects the stromal layer, beginning in childhood. Granular deposits within the cornea cause visual impairment, and treatment may require surgical intervention.
Macular Dystrophy
Affects the stromal layer, leading to opacity and vision loss. Treatment typically involves a corneal transplant.
Symptoms of Corneal Dystrophy
The symptoms of Corneal Dystrophy vary widely depending on the specific type and severity of the disorder. Common symptoms across different forms of Corneal Dystrophy may include:
- Blurry Vision: Accumulations in the cornea can scatter light, leading to blurred or distorted vision.
- Glare or Halos: Some individuals may experience increased sensitivity to light, causing glare or halos around lights.
- Pain or Discomfort: Corneal erosions, a common feature in some dystrophies, can cause significant pain or a gritty sensation in the eyes.
- Clouding of the Cornea: This can cause a decrease in visual clarity and might progress to significant vision loss in severe cases.
- Color Changes in the Cornea: Certain dystrophies may lead to visible changes in the color or transparency of the cornea.
- Frequent Changes in Prescription: Some individuals might notice a recurrent need to update their prescription for glasses or contact lenses.
The onset and progression of these symptoms can be gradual or sudden, and they may remain stable or worsen over time. Monitoring symptoms with regular eye check-ups and seeking prompt medical attention if symptoms develop or change is essential for managing Corneal Dystrophy effectively.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Who Does Corneal Dystrophy Affect?
Corneal Dystrophy can affect individuals of all ages, genders, and ethnic backgrounds, though the prevalence and manifestation may vary depending on the specific type of dystrophy and individual factors.
- Age Factor: Some types of Corneal Dystrophy may manifest in childhood, while others may not become apparent until later in life. The age of onset can vary widely.
- Genetic Factors: Many Corneal Dystrophies have a genetic component, meaning that they can run in families. A family history of Corneal Dystrophy might increase an individual’s risk.
- Gender Differences: Certain forms of Corneal Dystrophy may show differences in occurrence or severity between males and females.
- Environmental Factors: Though primarily a genetic disorder, environmental factors such as injury or other eye conditions might exacerbate or trigger the symptoms of Corneal Dystrophy in some individuals.
- Ethnic and Geographical Differences: The prevalence of specific types of Corneal Dystrophy may vary among different ethnic groups and geographical regions.
Understanding these factors can help in early diagnosis and management, especially in cases with a known family history of the condition. Regular eye check-ups and consultation with eye care professionals are essential for those at increased risk.
Diagnosing Corneal Dystrophy
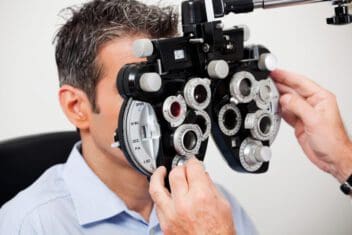
A routine eye examination can detect the development of corneal dystrophy. A full clinical examination is the best way to get an accurate diagnosis. This process will entail a patient history, especially determining if the patient has a family history of corneal dystrophy, and testing, like a slit lamp examination. With a slit lamp exam, a special microscope (a slit lamp) gives a doctor a high degree of magnification to study the buildup of particles and discover whether they are affecting corneal functions.
Certain genetic tests can diagnose the likelihood of specific corneal dystrophies developing, even before any symptoms present themselves.
Treating Corneal Dystrophy
How can corneal dystrophy be treated? Because there are many different types of the condition, treatment itself can vary.
People with asymptomatic corneal dystrophy (where there are no symptoms) or those who have mild symptoms might not require any treatment. Instead, it may be better for them to get regular checkups and examinations to see if the disease progresses to the point where treatment would be necessary.
Patients who require treatment might be given eye drops and ointments. For more serious cases, laser treatment and corneal transplants might be required. Recurrent corneal erosions (mentioned above) are usually dealt with via lubricating eye drops, antibiotics, ointments, or special contact lenses. If the erosions continue, a doctor might go a step further and perform corneal scraping or use excimer laser therapy, which can cut off abnormalities from the surface of the cornea (a procedure known as phototherapeutic keratectomy).
Patients who are in significant pain or suffering from vision loss might have to receive a corneal transplant. Also known as keratoplasties, these procedures are very effective in offering relief to patients who have advanced corneal dystrophy symptoms. Patients will likely have to continue receiving eye care for months after the procedure.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- What Is Corneal Dystrophy? The Corneal Dystrophy Foundation.
- Cornea. (March 2018). American Academy of Ophthalmology.
- Function of the Cornea. (December 2019). Very Well Health.
- Recurrent Corneal Erosion: A Comprehensive Review. (2019). Clinical Ophthalmology.
- Corneal Dystrophies. (June 2018). WebMD.
- What Is a Slit Lamp?. (April 2018). Healthline.
- How DNA Testing Screens for Corneal Dystrophy. (October 2013). Ophthalmology Times.
- Corneal Dystrophies. (February 23, 2009). Orphanet Journal of Rare Diseases.
- New Tools for Treating Corneal Dystrophy. (September 2005). Review of Ophthalmology.
- Cornea Transplant. (February 2018). Cleveland Clinic.
- Molecular Biology of Eye Disease. (2015). Progress in Molecular Biology and Translational Science.
- When and How to Treat EBMD. (September 2019). Review of Ophthalmology.
- Two Cases of Reis-Bücklers Corneal Dystrophy (Granular Corneal Dystrophy Type III) Caused by Spontaneous Mutations in the TGFBI Gene. (April 2006). JAMA Ophthalmology.
- Congenital Stromal Corneal Dystrophy. (November 2008). GeneReviews.
- Lattice Corneal Dystrophy. (June 2019). Medscape.
- Granular Corneal Dystrophy. Johns Hopkins Medicine.

Angelique Pillar, MD, is a cataract, cornea, and refractive surgeon with over a decade of post-fellowship experience and a proven track record of excellent surgical outcomes.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

