Treatment Breakthroughs for Macular Degeneration in 2022
Last Updated:
Macular degeneration is a top cause of vision loss, and at the moment, it is considered incurable. In 2022, researchers have been working hard to understand the cause of macular degeneration, and recently, have made strides in finding dry macular degeneration treatment breakthroughs and other treatments.
Table of Contents
Doctors can now use a new type of lens to help patients with macular degeneration, and that lens can magnify images before they reach the optic nerve, offering clearer vision. Vitamin therapy can also be helpful for people with some types of macular degeneration, although consumers should ensure that they are purchasing vitamins from a reputable supplier.

Injectable medications offer a form of therapy for some types of macular degeneration, although those injections must be repeated frequently.
Combining drug therapy with laser therapy is another way to control and even stop the spread of some forms of macular degeneration. New technology being developed in 2021 helps doctors to better use lasers to treat macular degeneration in 2022.
Researchers are also experimenting with the use of stem cells to help some patients with macular degeneration, although more research is required before this treatment can be recommended for everyone.
What Is Macular Degeneration?
The layer at the back of the eye, known as the retina, is responsible for our ability to see. The retina perceives images that move through the eye, and the retina transforms those images into electrical signals that can be processed by the brain.
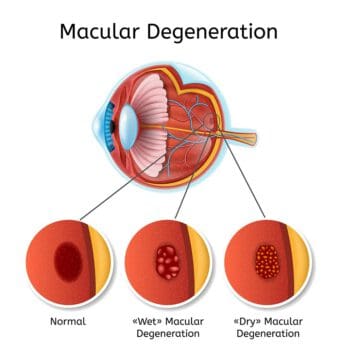
At the very center of the retina is the macula, and it’s responsible for our ability to see things at the center of our vision. When we focus our eyes on the words printed on a page in a book, for example, we are relying on the work of the macula.
Macular degeneration causes damage to the macula.
There are two forms of macular degeneration. The dry form is the most common, according to the American Macular Degeneration Foundation, as it represents about 90 percent of the cases of macular degeneration. This has led to an intensified focus on dry macular degeneration treatment breakthroughs.
This form of macular degeneration involves yellow deposits (known as drusen) sitting beneath the macula, causing thinning and dying of that vital tissue. This process takes time, and people may experience a slow and gradual deterioration of their ability to see things in the middle of the visual field.
People with the wet form of macular degeneration also lose the ability to see things in the middle of the field of vision, but their vision loss may happen quickly. This damage is caused by abnormal blood vessels growing beneath the macula.
When those blood vessels leak blood, rapid destruction of the macula takes hold. Lines may look wavy due to the buckling of the macula, and there may be clouds of vision loss in the center of the visual field.
Surgery With Lens Replacement
Some surgeons are experimenting with lens therapies for macular degeneration, thinking that making the lens work better might make the damage easier to move past.
During surgery, according to Mayo Clinic, surgeons insert a new lens that has the ability to magnify the field of vision. This allows the eye to use healthy parts of the macula when viewing an image, even without turning the head. More retinal cells are exposed to the light moving through the eye, which allows undamaged cells to take over for their damaged counterparts.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
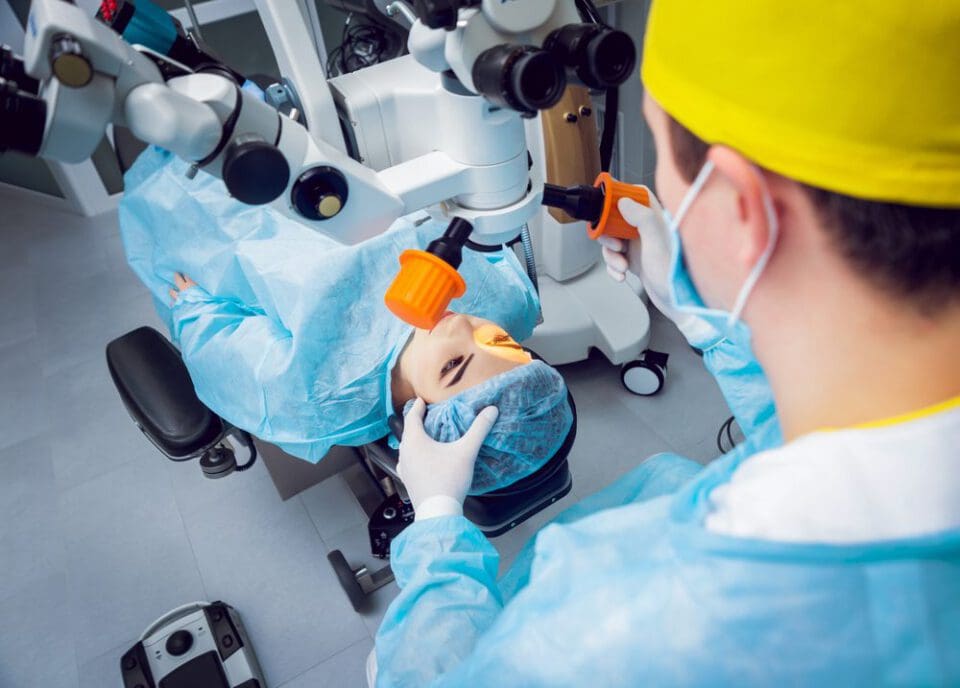
This surgery is not designed to halt the progression of macular degeneration, but it can help to make life with the disorder better.
As authors writing in Vision Aware explain, people prior to surgery may see only a black hole where a face should be. After surgery, they may be able to see eyes and a nose on the face in front of them. That shift may be small, but it may allow the person to recognize loved ones as well as read their facial expressions.
This is a new therapy for macular degeneration, and as researchers writing in Graefe’s Archive for Clinical and Experimental Ophthalmology point out, more research must be done before these lenses can be recommended for everyone. Since the lenses are so new, there is no real data about how well they work over the long term.
It’s unclear if complications persist years after surgery, for example, and it’s not certain how well people see in later years. Longer studies should offer that data.
Treatment with Diet
Eating various antioxidant-rich foods regularly can help with AMD management. Some studies indicate that a daily diet should include certain fruits and lightly cooked vegetables as part of any AMD treatment. Antioxidants fight off reactive molecules in the body called oxidants, which contribute to aging. Oxidants can accelerate macular degeneration in your eyes as you get older.
While vitamins A, C, and E can help protect eyes from this age-related vision problem, they’re not the only helpful antioxidants you should add to your diet. Consider incorporating sufficient supplies of carotenoids in your diet to boost your body’s defenses against AMD. These are antioxidants, too.
You should mix two important carotenoids, lutein and zeaxanthin, into your food consumption. The human body does not produce either, hence the need to add them as supplements.
Scientists believe that carotenoids, along with a lutein-derivative called meso-zeaxanthin, can help prevent macular damage. Without enough levels of these macular pigments, you may be at a higher risk of developing AMD.
Vegetables that contain lutein:
- Spinach
- Kale
- Red pepper
- Lettuce
- Broccoli
By eating a healthy diet that includes these foods every day, you can keep proper carotenoid levels to treat or manage AMD. Your body needs at least 10mg of lutein daily to provide adequate antioxidant protection.
Treatment With Vitamins
The macula is made up of sensitive tissues that rely on a mix of nutrients to stay healthy. An optimal diet can help to provide those cells with the nutrition they need, but many people simply don’t eat a diet that is rich in the right types of ingredients to help the eyes stay healthy. Vitamin supplements may help to fill the gap.
According to the National Eye Institute (NEI), researchers have performed two very important studies on the link between vitamins and macular degeneration. The first, concluded in 2001, allowed researchers to emerge with a vitamin formula. The second, concluded in 2013, included changes to the vitamin formulation.
The current dose recommended by NEI includes:
- Vitamin C: 500 mg
- Vitamin E: 400 IU
- Zinc oxide: 80 mg
- Lutein: 10 mg
- Copper: 2 mg
- Zeaxanthin: 2 mg
NEI reports that this supplementation is appropriate for people with intermediate or late forms of macular degeneration. It is not a cure for the disorder, and it will not help to restore sight that has been lost to the disorder. But the vitamins may help to slow the progression of the disease.
The American Academy of Ophthalmology reports that there are health risks associated with vitamin use, and it is important for people to talk with their doctors before they start taking vitamins to help with macular degeneration.
They also report that supplements alone cannot offer optimal nutrition. People should also make sure to eat a diet rich in leafy greens, as well as colorful fruits and vegetables.
The Bright Focus Foundation reports that it’s vital for people to ensure that the vitamins they are taking have the correct nutrient profile. Some vitamins sold as vital for eye health do not contain the ingredients researchers have linked to macular degeneration prevention. And others don’t contain the nutrients listed on the label.
It is important to buy them from a trusted source and ensure that the mix matches the one listed above.
Anti-VEGF Drugs

For people with the wet form of macular degeneration, doctors can use therapies to either remove or control the blood vessels growing beneath the eye. One such therapy uses anti-VEGF drugs.
Using this drug in the treatment of wet macular degeneration ensures that new, unusual blood vessels cannot grow beneath the macula of the eye, which can keep the disease from progressing.
According to the American Academy of Ophthalmology, doctors use a very small needle to deliver the drug into the tissues within the eye. The eye is numbed before the procedure, so patients don’t feel pain. It can be performed on an outpatient basis, so people can go home the same day the procedure is done.
The drug used in this therapy was originally designed to help people with cancer. In order to grow, cancer cells need a heavy dose of blood. The vessels that carry blood need the chemical VEGF to grow. The medication blocks the production of VEGF.
Unfortunately, as authors writing for The Lancet point out, people with macular degeneration need repeated injections of the medication, as the drug wears off in time. Each injection can be expensive, as can the procedure used to deliver the drug. Some insurance companies balk at the cost of this procedure, and they may not cover it for all patients.
Newer versions of the medications potentially last longer, requiring less frequent injections.
New delivery methods have been developed that may simplify the delivery of this medication.
In October 2021, the FDA approved the use of Genentech’s Susvimo, a port delivery system that is implanted into the eye. The implant is refillable, requiring a one-time outpatient surgery to place it and then refills every six months. Trials of the implant showed positive results for patients.
Gene Therapy
In 2022 and beyond, gene therapy may offer an alternative to ongoing injections of anti-VEGF drugs. The goal is to offer a one-time injection that stimulates the body to produce its own anti-VEGF properties.
Four different medications are being tested, including one for dry AMD and four for wet AMD.
With limited research, we don’t yet know the effectiveness of gene therapy, and the high price of the potential treatment may make it out of reach for most patients.
Photodynamic Therapy
Some medications work as soon as they hit the tissues within the body, but others need a form of activation in order to do their work. In photodynamic therapy, doctors use lasers to make an eye medication work to combat macular degeneration.
This treatment is appropriate for people with wet macular degeneration, according to Mayo Clinic. Doctors inject a drug into an arm vein, and then shine a laser on abnormal eye blood vessels. When the drug enters these blood vessels, it is activated by the laser, and the blood vessel is closed.
This is considered a revolutionary form of therapy, according to the American Macular Degeneration Foundation, as the laser used is not likely to damage healthy parts of the eye. It is focused only on damaged portions of the eye, amending what is broken while leaving everything else alone. It cannot cure macular degeneration or stop future damage, but it may help to preserve the vision people have now.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Stem Cell Implants
Doctors are also experimenting with the use of stem cells to assist with macular degeneration.
A stem cell is a type of cell that is undifferentiated, meaning that it can become any type of cell within the body. Doctors are looking for ways to use these cells to either replace or heal damaged cells that cause macular degeneration.
In one form of therapy, doctors line stem cells on a supportive structure, and they surgically implant that structure into the retina of the eye. In time, those stem cells grow into new retinal tissue, integrating with the tissue that is already there. Researchers feel the early results are promising, as people tend to tolerate the surgery well and one patient in four had an improvement in visual acuity.
In a second study published in the New England Journal of Medicine, researchers describe pulling stem cells from people’s bodies and using those cells on a supportive structure inserted into the eye. Instead of relying on embryonic stem cells, which makes some people uncomfortable, these researchers were using people’s own bodies to help them to see clearer. At one year after the procedure, researchers said, visual acuity hadn’t worsened. This seems to indicate the surgery helped to halt the progression of the disease.
It is important to note that both of these studies were small, and more must be done to determine how well this works in a larger group of people. But early results are certainly exciting.
Prozac
Research in 2021, which could be one of many dry macular degeneration treatment breakthroughs, showed that the antidepressant Prozac may slow the development of dry age-related macular degeneration.
An examination of insurance databases that contained more than 100 million Americans showed that those who were taking Prozac were less likely to develop dry AMD.
Though more studies are needed, Prozac (known generically as fluoxetine) may be used as a potential treatment for AMD in the future.
Can Macular Degeneration Be Reversed?
AMD reversal is still an active area of research, albeit with some promising findings. Currently, there’s no known cure for the condition.
Most treatment and management options available so far help to prevent further damage once AMD has developed. They’re still worth trying as they can improve vision in some patients.
A potential cure for age-related macular degeneration is HTRA1 protein augmentation. Scientists have studies augmentation therapy for more than a decade and are now starting to see promising signs of treatment.
HTRA1 Protein Augmentation
A team of scientists at the University of Utah Moran Eye Center started researching AMD reversal in the early 2000s. The most recent findings show that increasing levels of a protein called HTRA1 in the retina may help reverse AMD vision damage.
The team studied a group of people with certain genetic variants linked to the development of AMD. At advanced age, these candidates did not have a normal expression of the HTRA1 gene in certain areas of the eye.
In turn, individuals had a nearly 50-percent deficiency in the HTRA1 protein. The amount of this protein in the retina increases with age in normal eyes, instead of decreasing.
This compound contributes to the proper functioning of the retina. According to the study, augmentation therapy to restore healthy HTRA1 protein levels in affected eyes may cure AMD.
The potential treatment may also help slow the disease’s progression.
What Therapy Is Right for You?
When you’re living with macular degeneration, it’s vital to work with an eye doctor you can trust. We can connect you with that doctor. At NVISION, we have qualified and compassionate doctors who can explain your diagnosis and your treatment options. Contact us and find out more.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- What Is Macular Degeneration? American Macular Degeneration Foundation.
- Dry Macular Degeneration: Diagnosis and Treatment. (November 2018). Mayo Clinic.
- The Implantable Miniature Telescope (IMT) for End-Stage Age-Related Macular Degeneration. Vision Aware.
- Intraocular Lenses in Age-Related Macular Degeneration. (July 2017). Graefe’s Archive for Clinical and Experimental Ophthalmology.
- Facts About Age-Related Macular Degeneration. (November 2018). National Eye Institute.
- Vitamins for AMD. (May 2018). American Academy of Ophthalmology.
- Vitamins for Age-Related Macular Degeneration: Do You Have the Correct Formula? (March 2017). Bright Focus Foundation.
- How Is AMD Diagnosed and Treated? (May 2018). American Academy of Ophthalmology.
- What Is Avastin? (May 2018). American Academy of Ophthalmology.
- Age-Related Macular Degeneration: Treatment at What Cost? (September 2018). The Lancet.
- Wet Macular Degeneration: Diagnosis and Treatment. (December 2015). Mayo Clinic.
- New Treatments for Age-Related Macular Degeneration. (February 2021). American Academy of Ophthalmologists.
- Macular Degeneration Treatments. American Macular Degeneration Foundation.
- New Retinal Implant Produces Hope of Cure for Macular Degeneration. (April 2018). Healthline.
- Autologous Induced Stem-Cell-Derived Retinal Cells for Macular Degeneration. (March 2017). The New England Journal of Medicine.
- Advancing a Stem Cell Therapy for Age-Related Macular Degeneration. (2020). Current Stem Cell Research & Therapy.
- Identification of Fluoxetine as a Direct NLRP3 Inhibitor to Treat Atrophic Macular Degeneration. (October 2021). Proceedings of the National Academy of Sciences of the United States of America.
- Pharma FDA Greenlights Genentech’s Eye Implant for Macular Degeneration. Will It Be a Tough Sell? (October 2021). Fierce Pharma.
- FDA Approves New Injection Brolucizumab (Beovu ) for Wet AMD. (October 2019). Medscape.
- New Tech Could Treat Retinal Diseases That Affect Millions Worldwide. (May 2021). Troy Media.
- Nutrition. Macular Society.
- The University of Utah Moran Eye Center. (July 2021). Researchers: Htra1 Augmentation is Potential Therapy for Age-Related Macular Degeneration.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

