
Medically Reviewed by Roberto Roizenblatt, M.D. NVISION Surgeon
Scleral Buckle Surgery: Costs & Preparation Guide
Last Updated:

Medically Reviewed by Roberto Roizenblatt, M.D. NVISION Surgeon
The retina is the small layer of tissue in the back of the eye that processes light. It uses the optic nerve to send visual images and information to the brain.
Table of Contents
The retina can be torn or completely detached. This often requires surgical treatment to prevent permanent vision loss.
A scleral buckle surgery attaches a small synthetic band on the white part of the eye, called the sclera, to change the shape of the eye. This helps to push the retina back in place to heal the tear or detachment.
Scleral buckle surgeries have a success rate that is over 90 percent. There are some risks associated with the surgery, and additional surgeries are sometimes needed to correct vision.
Scleral buckle surgery is deemed by insurance a medically necessary procedure. It is performed at the hospital or surgery center under anesthesia.
You will usually need at least several months to recover after a scleral buckle surgery.
Overall, a scleral buckle surgery can help to repair a torn or detached retina. It can save you from further damage to your vision.
When Scleral Buckle Surgery Is Needed
Scleral Buckle surgery has been used for decades to repair a retinal detachment.
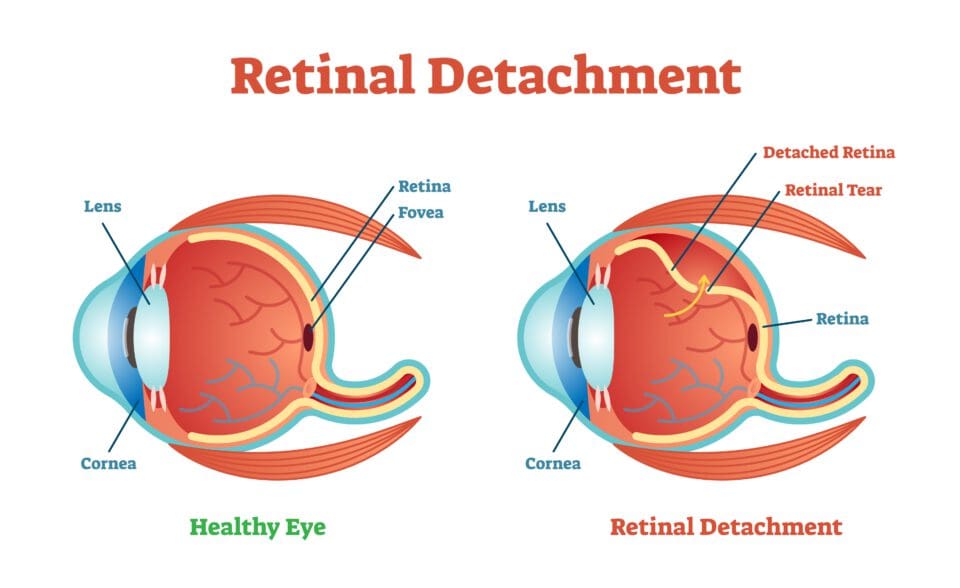
Patients with retinal detachment often don’t complain about pain but may experience some symptoms. Primary symptoms include:
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
- Partial loss of vision
- Blurred vision
- Sudden light flashes that appear when looking to the side
- Sudden floaters in the field of vision, which can impair vision
Retinal detachment can occur in patients with the following risks:
- Trauma to the eye
- Advanced age, 50 years and above
- Diabetes mellitus patients
- Cataract removal surgery complications
- Family history of retinal detachment
- Extreme myopia, causing a lot of strain on the eye
- Posterior vitreous detachment, especially in old adults
The Ins & Outs of Scleral Buckle Surgery
Scleral buckle surgery is a common method for treating retinal detachments and sometimes tears as well. The surgery is most commonly performed under general or local anesthesia at a hospital by a specialty trained surgeon.
During the surgery, the retina is pushed back into place. A small flexible band or sponge, usually made out of silicone or another synthetic material, is attached to the white part of the eye (the sclera). This band alters the shape of the eye and slightly pushes the eyeball down into the retina, allowing it to reattach and fixing any breaks.
The scleral buckle slightly changes the circumference of the eye. The band is usually permanently attached and covered by the skin of the eye so it is not visible.
Cryopexy or laser photocoagulation may also be performed at the time of a scleral buckling procedure in order to prevent possible repeat tears. Cryopexy involves freezing the outer surface of the eye, while laser photocoagulation burns it. Both are meant to create scar tissue that help to seal possible retinal breaks and tears.
Fluid buildup behind the retina may also be removed during surgery.
The main goal of treatment for retinal detachment is to seal tears or breaks and reattach the retina to the back wall of the eye. Scleral buckle surgery is often a good procedure for this.

Pros & Cons of Scleral Buckle Surgery
Most of the time, a scleral buckle surgery is considered to be successful in reattaching the retina and sealing up tears.
Therefore, the following are some risk factors associated with it:
- Bleeding
- Double vision
- Scarring of the retina and redetachment
- Infection
- Increased eye pressure
- Vision loss
Discuss all of the potential complications, as well as benefits, of a scleral buckle procedure with your doctor beforehand.
Preparing for Your Surgery
Be sure to arrange for someone to take you home as scleral buckle surgery is usually a same-day procedure.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Scleral Buckle Recovery

After the surgical procedure, the doctor will place an eye patch over your eye to protect it for at least a day. You will likely meet with your surgeon or someone on the medical team within the first day or so after surgery for a follow-up visit.
You will be sore and likely have redness and swelling on and around the eye for the first several weeks after surgery. You will be given eye drops that you will need to apply for several weeks to help with healing.
You may want to take medications for the pain.
If you experience increasing pain and swelling, discharge from the eye, or decreased vision, let your doctor know right away.
Alternatives to Scleral Buckle Surgery
Your eye surgeon will prescribe the best procedure for retinal detachment that suits your condition. If a Scleral Buckle procedure isn’t viable, your doctor may alert you to a couple of alternatives. The first is a vitrectomy, and the second is pneumatic retinopexy, or a combined procedure.
Vitrectomy
Vitrectomy is an alternative surgery used to treat retina and vitreous eye problems. During the procedure, your eye surgeon removes and replaces the vitreous with another solution. Any tears or holes in the retina are also repaired during the surgery.
Pneumatic Retinopexy
Pneumatic Retinopexy is an outpatient procedure used to repair some types of retinal detachments. During the procedure, the eye is injected with a gas bubble to gently push the retina into position. The procedure is done alongside photocoagulation or freezing therapy to seal the area around it.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Scleral Buckle Surgery for Primary Retinal Detachment Without Posterior Vitreous Detachment. (November 2016). Retina.
- Facts About Retinal Detachment. (October 2009). National Eye Institute (NEI).
- Scleral Buckle. (2019). Mayo Clinic.
- Scleral Buckle for Rhegmatogenous Retinal Detachment. (October 2015). American Academy of Ophthalmology (AAO).
- Retinal Detachment. (2019). The American Society of Retina Specialists.
- Cost Comparison of Scleral Buckle Versus Vitrectomy for Rhegmatogenous Retinal Detachment Repair. (September 2018). American Journal of Ophthalmology.
- Retinal Detachment. (March 2019). Mayo Clinic.
- A Review of Retinal Detachment Repair. (January 2019). Review of Ophthalmology.
- Anatomic Success of Scleral Buckling for Rhegmatogenous Retinal Detachment- a Retrospective Study of 524 Cases. (March 2010). Ophthalmologica.
- Cataract surgery. (August 31, 2019). Mayo Clinic.
- Vitrectomy for retinal detachment. (December 23, 2020). National Eye Institute.
- Comparison between pneumatic retinopexy and Scleral Buckle for retinal detachment repair. (November 1, 2017). Ophthalmic Surgery, Lasers and Imaging Retinal.

Dr. Roberto Roizenblatt received his medical degree from the University of Sao Paulo in Brazil. He went on to complete an internship in Internal Medicine at Jacobi Medical Center in New York, followed by successfully completing two residencies in ophthalmology at the Federal University of Sao Paulo and later at the University of California, Irvine.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

