
Medically Reviewed by Tom Tooma, M.D., Founder/Medical Director NVISION Surgeon
Bumps Under the Eyes: Types & How to Treat Them
Home / Eye Health and Preventive Care /
Last Updated:

Medically Reviewed by Tom Tooma, M.D., Founder/Medical Director NVISION Surgeon
Bumps under the eyes and lower eyelid have several causes, some of them no cause for concern. However, there are a few serious conditions which can require treatment, and some causes can even pose a threat to your eyesight. Learn the difference and when to be concerned here.
Various causes of under-eye bumps include milia, styes, and chalazia. Milia are mostly harmless, sometimes referred to as “chicken skin” due to appearance. Styes form from infected eyelash glands and usually go away by themselves in a few days. Chalazia are a more serious infection which requires medical attention. Almost all blemishes around the eye area can be addressed by practicing sound eye hygiene.
Table of Contents
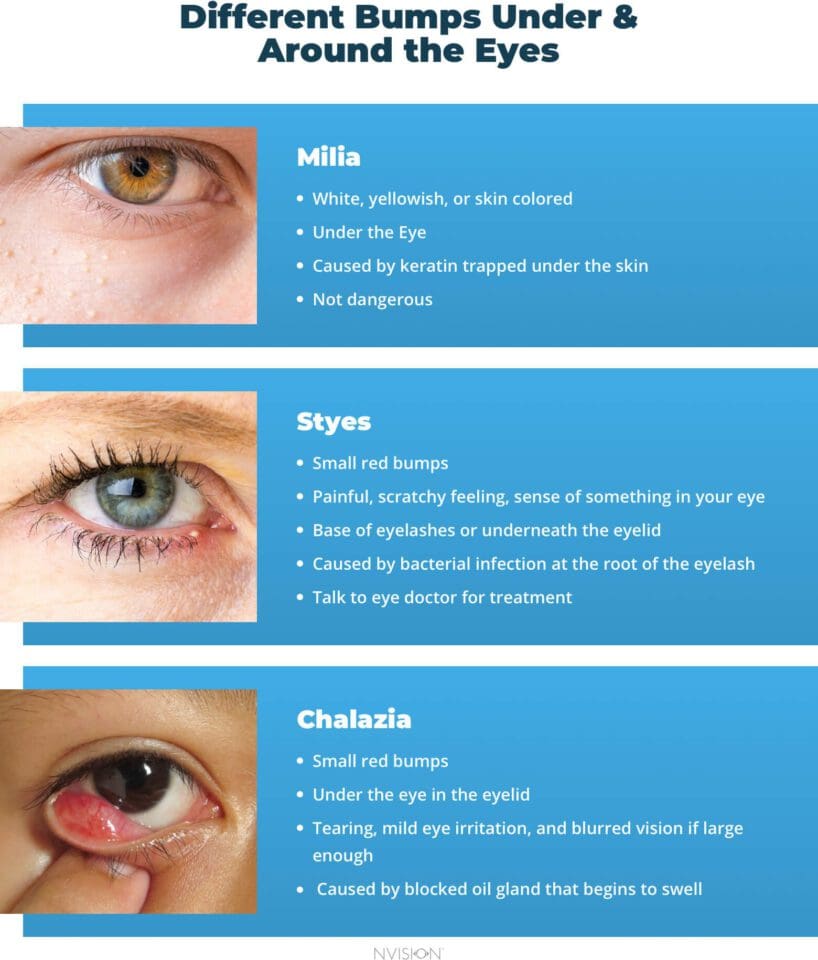
Causes of Bumps Under the Eyes
Milia Bumps
Milia is a very common condition and not at all dangerous. Milia are small bumps that can appear anywhere on the skin, often under the eyes. These bumps are formed by keratin that is trapped under the skin by a clogged sweat gland. Milia can be white, yellowish, or skin colored. Some people call milia milk spots due to their whitish appearance. These bumps are small spots or cysts, and they are not a type of acne.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Styes
Styes are small red bumps that appear along the eyelash line on the upper or lower eyelid. They can also rarely form inside the eyelid. Styes are typically caused by a bacterial infection at the root of the eyelash. They can be painful and exhibit redness and swelling, but can also go away in a day or two on their own.
Styes may have some of these additional symptoms:
- A painful red bump at the base of your eyelashes
- A spot of pus at the center of the bump
- The sense of something being in your eye
- Scratchy feeling in your eye
- Sensitivity to light
- Crusty eyelid
- Tearing of the infected eye
Anyone can develop a stye under their eye; they are so common that almost everyone gets them. People who have blepharitis and certain skin conditions, such as rosacea or seborrheic dermatitis, are at an increased risk for developing styes. Additionally, medical problems like diabetes increase the risk of styes.
Styes can go away on their own, and can even be treated at home with a warm compress over the eye. But if a stye sticks around for a few days, you will want to consult a doctor. Some infections can get out of hand, spread to the rest of the eyelid and eye area, or change into a more serious infection.
Medical intervention for a stye may be as simple as treating with local antibiotics, or can involve surgical removal. If you are prone to frequent styes, you might have underlying medical issues.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Chalazia
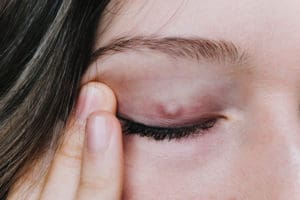
Chalazia are very hard to miss. They can form a red lump in the eyelid tissue of both the upper and lower eyelids, either on the outside or inside of the eyelid. Unlike styes, chalazia are not typically painful but do grow much larger. Chalazia are not caused by a bacterial infection, but rather a blocked oil gland.
Chalazia can have these accompanying symptoms:
- A red, tender, swollen bump on the eye
- Tearing
- Mild eye irritation
- Blurred vision, when the chalazion is large enough
Chalazia can get quite large, even enough to partially obstruct vision.
Like styes, a minor chalazia may be treated at home with a warm compress. If they do not clear up within a week, seek medical attention. Doctor’s treatments for chalazia may require surgical removal, or steroid shots to promote drainage.
Treatment and Prevention
While you can attempt to self-diagnose bumps under your eyes, there is a chance you won’t identify the bumps correctly. This is why it’s generally best to see a doctor to confirm your suspicions.
At-home measures, such as applying warm compresses and following proper eye care hygiene steps, can promote general eye health.
Ophthalmologists and dermatologists stress that patients should not attempt to “pop” or squeeze milia, styes, or chalazia. Doing so can damage the skin, increase your risk of infection, and cause scarring.
When to See a Doctor
Seek medical attention in the case of styes or chalazia if it becomes painful, lasts for longer than a week, or does not respond to warm compress treatment. Also seek medical attention if the affected area oozes discharge, obscures your vision, or appears to spread.
Virtually nothing but cosmetic surgery can be done about milia, which is quite common in everyone and becomes more common with aging.
Prevention
While it is not possible to completely prevent styes and chalazia, practicing good facial hygiene is an important step you can take to minimize them. Practice these tips, and you’ll minimize the bumps around your eyelid area:
- Good hygiene: Always wash your hands thoroughly before touching your eyes.
- Remove eye makeup: Cleanse your face every night, carefully removing all makeup from around your eyes. Never go to bed with makeup on.
- Use clean towels and washcloths: Never use a dirty towel around your eyes.
- Replace outdated makeup: Bacteria can form on old makeup. Aim to replace all eye makeup every six months.
- Never share eye makeup with anyone else: You can pass bacteria around from person to person easily.
FAQS
Can I wear makeup to cover the bumps?
Depending on the type of bumps under the eye, you can sometimes apply makeup to camouflage them for work or social engagements.
If you have a stye or chalazia, you should ideally not apply makeup to it. If you can take a break from eye makeup until the area heals, this is the best approach.
Eye makeup can carry bacteria and spread a stye to the other eye. If you have to apply makeup for a particular engagement, use a non-comedogenic makeup that won’t clog your pores. And clean your makeup brushes thoroughly before and after applying to ensure you aren’t spreading bacteria.
You can cover milia with makeup, but it’s best to use oil-free varieties to avoid further clogging pores. Try to avoid anything heavy in the area.
How can I prevent milia under the eyes?
The best way to prevent milia is to fully cleanse your face daily, paying particular attention to the area under your eyes. Make sure to fully remove makeup.
Don’t use oily eye makeup removers, which can trigger milia. This is because they often leave oily residue under the eyes.
Gently exfoliate under your eyes. This can greatly reduce existing milia and prevent future problems.
Talk to your dermatologist about the best serums, creams, or lotions to use in the area. Some doctors recommend incorporating retinol or AHA or BHA exfoliators into your routine. Generally, you should stay aware from heavy creams.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Chalazion. American Optometric Association
- Milia. (March 2017). Medscape.
- What Are Chalazia and Styes? (August 2019). American Academy of Ophthalmology.
- What Are Milia — And How to Get Rid of Them. (August 2018). USF Health, Dermatology & Cutaneous Surgery.
- Chalazion. Cleveland Clinic.
- Here’s How to Wear Makeup With a Stye. (April 2016). Bustle.
- Milia: What They Are, and How to Remove Them. (October 2017). Teen Vogue.
- SkinSchool: Milia Causes and Treatment Options. (January 2021). Harper’s Bazaar.

Dr. Tooma, the founder of NVISION® Eye Centers, has performed well over 130,000 LASIK surgeries, making him the most experienced LASIK surgeon in the Western United States.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.


