
Medically Reviewed by Leon G. Partamian, M.D. NVISION Surgeon
How Long Does Traumatic Iritis Take to Heal?
Home / Eye Conditions & Eye Diseases / What Is Uveitis? /
Last Updated:

Medically Reviewed by Leon G. Partamian, M.D. NVISION Surgeon
It takes traumatic iritis about a week to heal, though exact treatment times vary according to the severity of the issue.
Traumatic iritis is a specific type of iritis, or inflammation of the colored part of the eye, which is caused by trauma. Impact from a bat, a car accident, and a flying object on a construction site are all common causes of this injury.
Wearing eye protection for sports, dangerous jobs, or risky hobbies will help to reduce your risk of traumatic iritis. If you are hit in the head or the eye, go to an ophthalmologist as soon as possible for diagnosis and treatment.
Treatment includes special eye drops to dilate the pupils, which relieves pressure; corticosteroids to reduce tissue inflammation; and general rest at home. This care should continue for about one week before you see your doctor for a follow-up appointment.
Traumatic Iritis: What It Is & How It Heals
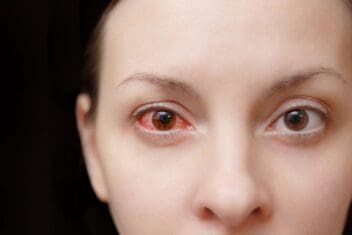
Traumatic iritis is a type of iritis, or inflammation of the colored part of the eye, due to trauma like being hit or scratched. This is a type of uveitis, so traumatic iritis is also referred to as anterior uveitis. Sometimes, a combination of inflammation of the iris and the ciliary body is called iridocyclitis.
Regardless of how the condition is diagnosed, it can be serious. Without appropriate treatment and time to heal, it can cause lasting vision loss and might even trigger glaucoma, or high fluid pressure in the eye that leads to blindness from pressure on the optic nerve.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
If you experience a blow to the head or eye, you may develop this inflammation. Without proper rest and treatment, it can lead to permanent vision impairment. Fortunately, most people respond well to treatment, which includes resting your eyes as much as possible. Following the prescribed course of treatment means you are very likely to reduce pain and heal in about a week.
Risks & Causes of Traumatic Iritis
Trauma to the eye is the leading cause of iritis or anterior uveitis.
- A dozen out of every 100,000 people in the United States develop traumatic iritis.
- About 90 percent of uveitis cases are iritis, and about 20 percent of iritis incidents are traumatic iritis.
- Younger people are at greater risk than older adults.
- Men tend to develop traumatic iritis more than women.
Common causes of traumatic iritis include:
- Falling and hitting the eye or eye socket.
- An object like a bat or ball impacting the eye.
- Fireworks being set off too close to the face.
- Car accidents.
- Pellet gun projectiles.
If you work with tools or equipment that might cause eye damage, like working in a wood shop or playing professional sports, it is vital to wear eye protection to reduce the risk of traumatic iritis. It is also important to take eye safety precautions for certain types of work and hobbies, including sports, hunting, or using shop tools.
Symptoms of traumatic iritis include:

- Swelling or higher presence of white blood cells in the anterior chamber of the eye.
- Pain associated with light, including average room light.
- Floaters, or seeing more spots in your vision.
- Ciliary flush, or a ring of redness around the iris.
- Hypopyon, or accumulation of pus seen as a white spot at the bottom of the iris.
- Vossius ring, or a ring of opaqueness at the back of the lens from eye trauma.
- General ocular pain as your eye heals, typically throbbing or dull aching, which should not last more than three days after the trauma.
- Decreased ability to see clearly.
Sometimes, traumatic iritis has similar symptoms to a corneal abrasion, so going to an ophthalmologist for a full examination is important to getting the right treatment. Your ophthalmologist will also rule out any history of eye problems, like high fluid pressure that might cause glaucoma. By ruling out any other cause, you can get the best possible treatment.
If you are hit in the head or directly in the eye, you should see a doctor or ophthalmologist as soon as possible to ensure there is no serious head or eye injury, even if you do not immediately experience side effects or vision changes. If you develop vision problems or eye pain after seeing a doctor, be sure to let them know about these changes so they can keep your vision as healthy as possible.
Typical recommendations include attending a follow-up eye care visit within a week after a traumatic event, so your eye doctor can monitor your eyes’ healing progress.
Medical Treatments for Traumatic Iritis
After being diagnosed with traumatic iritis, the first step is for your ophthalmologist to dilate your pupil. The iris consists of fibers and muscles around the pupil that telescope the area to allow more or less light to hit the retina. By dilating your pupils, your eye doctor will relieve some pain and reduce eye spasms. This can also prevent eye tissue from sticking together.
You may need to use dilating eye drops for a few days. These will increase your sensitivity to light, so plan to remain at home in a darkened room to reduce eye pain until they wear off.

You are also likely to receive a prescription for a corticosteroid, which reduces tissue inflammation. You may take this medication as many as four times per day, and you may experience side effects like increased energy, anxiety, and aggression.
Work with your doctor to taper yourself off steroids once they are no longer needed. Quitting this medication suddenly can cause unpleasant withdrawal symptoms and might make your eye pain feel worse.
Although your eyes may hurt, it will be important to avoid aspirin and other nonsteroidal anti-inflammatory drugs (NSAIDs). These medications can thin your blood, which can increase the risk of bleeding at the site of the trauma. This might slow down the healing process for some people, so talk to your eye doctor before you take any medication.
By following your ophthalmologist’s advice, you will see noticeable improvements in your vision in about a week, which will be when your first checkup is scheduled. You should also schedule a follow-up appointment about a month after that, to ensure that healing is continuing as it should.
If you experience any side effects from medications or the trauma, along with any new symptoms or vision changes, let your ophthalmologist know. Complications can develop, so it’s important that your eye doctor is aware. They can help you manage any problems without long-term effects on your vision.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Traumatic Iritis. (September 2020). American Academy of Ophthalmology (AAO).
- Iritis. (October 2020). Guy’s and St. Thomas’ NHS Foundation Trust.
- Traumatic Iritis and Chemical Iritis. (September 2020). Merck Manual.
- Traumatic Uveitis in the Mid-Atlantic United States. (October 2015). Clinical Ophthalmology.
- Traumatic Uveitis Following Blunt Ocular Trauma and Complications. (September 2016). Investigative Ophthalmology & Visual Science.
- Recognizing and Treating Eye Injuries. (February 2019). American Academy of Ophthalmology (AAO).
- Evaluation of Traumatic Uveitis in the Emergency Department. (April-June 2019). Advanced Emergency Nursing Journal.

Dr. Leon Partamian is a renowned glaucoma specialist with decades of experience in both clinical practice and academic medicine.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

