Does Uveitis Cause Blindness? (How & Why)
Home / Eye Conditions & Eye Diseases / What Is Uveitis? /
Last Updated:
Table of Contents
Uveitis refers to a variety of conditions that cause inflammation of the inside of the eye. If left untreated, it can result in vision loss and blindness.
The uvea is part of the eye that consists of the iris, pars plana, choroid, and the ciliary body. The uveal also has many blood vessels that nourish the eye.
Different forms of uveitis affect the different regions of the uvea. Anterior uveitis affects the front of the eye; intermediate uveitis affects the middle of the eye, and posterior uveitis affects the back of the eye, near the retina. Panuveitis affects all three regions of the uvea.
The exact cause of uveitis is unknown, although some conditions and infections, especially inflammatory conditions, are linked to an increased risk of its occurrence.
Symptoms of uveitis include vision problems, eye pain, eye floaters, and eye redness.
Early detection and treatment of uveitis are important for reducing the risk of dangerous complications, which may include glaucoma and vision loss. Treatments may include antiviral medications, steroids, immunosuppressants, and eye drops to dilate the pupil.
What Is Uveitis & Can It Cause Blindness?
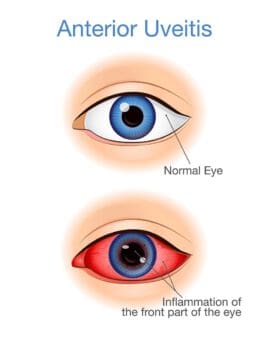
The middle layer of the eye is the uvea. Uveitis is a general term that refers to a variety of conditions that cause inflammation to the uvea as well as to any inside part of the eye.
Uveitis may be very painful and cause eye tissue swelling and damage. If left untreated, it can result in vision loss and even complete blindness due to complications, glaucoma, or retinal detachment.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Uveitis is the fifth leading cause of vision loss in the U.S. Although uveitis can affect people of all ages, it most commonly occurs in people between the ages of 20 and 60.
What Makes Up the Uvea?
The uvea — also called the uveal layer, the uveal coat, the uveal tunic, or the uveal tract — is a part of the eye that consists of:
- The iris. It surrounds the pupil and is the colored part of the eye.
- The pars plana. This is a single layer of the eye.
- The choroid. This thin white layer is between the white of the eye (the sclera) and the retina at the back of the eye.
- The ciliary body. This muscle is behind the iris, connecting the iris to the choroid.
The uvea has many blood vessels that provide nourishment and oxygen supply to the eye. Uveitis can damage these essential eye tissues, resulting in vision loss.
What Are the Different Types of Uveitis?
Different forms of uveitis affect the various components of the uvea. They are usually classified by where they occur in the eye.
- Anterior uveitis, also called iritis (inflammation of the iris), is the most common type of uveitis, and it occurs in the front of the eye. This form of uveitis usually occurs in young or middle-aged people, and it may affect only one eye. It is sometimes associated with lung, skin, gastrointestinal, and rheumatologic disorders, as well as infectious diseases. Symptoms of anterior uveitis can occur suddenly and last up to eight weeks.
- Intermediate uveitis affects the fluid-filled space within the eye, called the vitreous. Intermediate uveitis affects mostly young people and is associated with sarcoidosis and multiple sclerosis. Symptoms can last anywhere from a few weeks to years. They may go through cycles of improving and then getting worse.
- Posterior uveitis occurs in the back of the eye and may involve both the retina and the choroid. Although it is the least common form of uveitis, it has many infectious and noninfectious causes. Symptoms may gradually get worse and last for years.
- Panuveitis describes all three parts of the eye being affected by inflammation. Forms of panuveitis, such as Behcet’s disease, are extremely serious and can cause significant damage to the retina.
Intermediate, posterior, and panuveitis are the most serious forms of uveitis. They can lead to blindness or vision loss if left untreated
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
What Causes Uveitis?
The exact cause of uveitis is unknown, although some conditions and infections are linked to an increased risk of its occurrence. These include:

- Autoimmune disorders that include juvenile arthritis, psoriasis, and rheumatoid arthritis.
- Inflammatory conditions like Cohn’s disease and ulcerative colitis.
- Viruses and infections that surpass the immune system, including HIV/AIDS, herpes simplex and zoster (shingles), Lyme disease, syphilis, and tuberculosis.
- Infections inside the eye. Uveitis may occur as an immune system response.
- Eye trauma.
Uveitis may be caused by problems or diseases in the eye, or it may be caused by an inflammatory disease affecting other parts of the body.
What Are Symptoms of Uveitis?
The symptoms of uveitis are unpredictable and may develop gradually or rapidly.
Symptoms will vary depending upon the type of uveitis (its location in the eye). They may include the following:
- Blurred or cloudy vision
- Sudden changes in vision
- Floaters, which are spots in the eye that float around the field of vision
- Eye pain
- Eye redness
- Sensitivity to light
- Headaches
- A change in the appearance or color of the pupil
What Treatment Is Available for Uveitis?
The treatment for uveitis will depend on the severity of the inflammation and where inside the eye it is located. The earlier uveitis is detected, the easier it will be to treat.
Untreated uveitis can result in complications and more serious eye diseases, including cataracts, glaucoma, retinal edema, and permanent vision loss.
Treatment options include:
- Antibiotic and antiviral medications, which will be used if infection is present.
- Steroids, or corticosteroid medications, to treat inflammation. Corticosteroid medications are provided via eye drop, tablet, or injection to the eye. Before use, thorough testing (usually conducted with a fluorescent dye test) must be done to ensure no corneal ulcers are present.
- Immunosuppressants in cases of extreme symptoms, in which loss of vision is a risk. Immunosuppressants may also be used if the patient hasn’t responded to other medications.
- Mydriatic eye drops. These dilate the pupil to prevent muscle spasms and help with healing of the eye as well as eye pain. They stop the pupil from attaching to the lens and causing damage or irritation.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- What Is Uveitis? (April 22, 2018). American Academy of Ophthalmology.
- Facts About Uveitis. (August 2011) National Eye Institute.
- Uveitis: What You Need to Know. (March 7, 2017). Medical News Today.
- Anterior Uveitis. American Optometric Association
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

