
Medically Reviewed by Duna Raoof, M.D. NVISION Surgeon
Fixing a Lazy Eye: Your Best Options in 2025
Home / Eye Conditions & Eye Diseases /
Last Updated:

Medically Reviewed by Duna Raoof, M.D. NVISION Surgeon
To fix a lazy eye, you have a few options in 2025. Your optometrist may recommend surgery. Otherwise, they will focus on noninvasive treatments like eye patches or eye drops.
Table of Contents
Lazy eye, known also by the medical term amblyopia, is a condition in which one eye loses vision due to serious refractive error, occlusion of the eye, or problems with the eye muscles (strabismus), so good visual signals are not sent to the brain. In turn, the brain focuses on the signals from the dominant eye, so the non-dominant eye atrophies.
Amblyopia is diagnosed most often in children, and treatment can begin from infancy to age 7. By the time the child is 8 years old, vision is less likely to respond to treatments, surgical or nonsurgical.
While much of the focus on treating lazy eye, or amblyopia, is often placed on children, adults too can seek solutions for this issue. Understanding how to fix lazy eyes in adults may mean learning more about surgical options. The surgical procedures to correct strabismus, for instance, can be performed in adults, and are combined with non-surgical treatments to increase the chances of improvement.
What Is Lazy Eye?
The colloquial term lazy eye refers to a condition known among optometrists and ophthalmologists as amblyopia. This condition typically begins just after birth, and it continues to develop up to 7 years old.
About 2 percent of all children in the United States are affected by amblyopia. It is the most common cause of partial or total blindness in one eye in the U.S. Lazy eye rarely affects both eyes.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Although lazy eye can result in partial blindness, which impacts overall quality of life, diagnosing it early is fairly simple. In 2025, there are several treatments that can improve eye strength and prevent blindness.
- One eye that wanders inward or outward.
- Eyes that do not seem to work together to focus on objects.
- Trouble with depth perception.
- Squinting or shutting one eye to see better or force the eyes to work together.
- Tilting the head.
- Abnormal results on vision screen tests.
The underlying issue leading to lazy eye is not a problem with the structures of the eye itself, but the connection to the brain. If a child has one eye that does not see as well as the other, the brain will focus on interpreting signals from the dominant eye, and the non-dominant eye will slowly lose its ability to see.
While many instances of lazy eye are obvious due to strabismus, there are several cases in young children in which the condition is not immediately obvious. To reduce the risk of amblyopia becoming more serious, a complete eye exam is recommended for children starting between the ages of 3 and 5.
Why Does Lazy Eye Develop?
There are several causes of lazy eye.
- Strabismus (muscle imbalance): This is an imbalance in muscle strength between the eyes, so one eye is able to move more freely than the other. This leads the eyes to cross or turn out away from each other. It prevents the eyes from tracking in a coordinated way.
- Refractive anisometropia (difference in vision sharpness between the eyes): This involves significantly different refractive errors in each eye. It is often due to farsightedness, but it is sometimes caused by nearsightedness or astigmatism. It can lead to one eye becoming stronger than the other.
- Deprivation: An early cataract, cloudiness on the cornea, or another visual problem in one eye can lead the other eye to quickly become stronger. Deprivation amblyopia in an infant is considered a serious risk and requires immediate treatment to prevent blindness.
Treatments for the Causes of Lazy Eye
Fortunately, there are treatments that improve eye coordination and strengthen the muscles of the eyes. Treatments are more effective the earlier the condition is diagnosed. After a child reaches 8 years old, on average, the likelihood of vision improvement with treatment drops significantly.
Nonsurgical Treatments
There are several nonsurgical approaches to treating lazy eye. If amblyopia is due to an underlying refractive error, the child will receive a prescription for glasses, so the affected eye can get used to seeing the world more clearly, which can improve its overall function. If the cause of amblyopia is strabismus, additional treatments

- Eye patches or eye occlusion. A patch is placed over the “good” eye, forcing the muscles in the lazy eye to develop greater strength. Since the brain still receives information from that eye, especially in younger children, it will not ignore the signals and will begin to interpret them. Treatment length will vary depending on how serious the eye’s turn was, how long it had been that way, and how old the child is. Eye patches should be comfortable and remain in place with a child’s regular level of physical activity. The child should not be able to see around the edges, including seeing light filtered through. There are decorated patches available for children to encourage them to wear the patch and help them have fun during treatment. It is important to encourage your child to leave the patch in place. If your child already has eyeglasses, there are patches that attach to the lens of one side of the glass. This may be a second stage in the treatment process after the non-dominant eye has regained some strength. These types of patches are not good for children who are new to treatment.
- Atropine eye drops. These may be applied to blur vision in the “good” eye. Like the eye patch, this forces the non-dominant eye to become stronger. Signals between that eye and the brain will become stronger. Drops are usually easier for the child than wearing an eye patch.
- Vision exercises. Games and exercises designed to improve vision can strengthen the muscles of the affected eye. Games and activities include coloring in special workbooks, dot-to-dot drawing, word games, or using building blocks, depending on how old the child is. Home-based exercises may be recommended after the weaker eye has regained some strength. These may be done in combination with other treatments.
Surgical Treatments
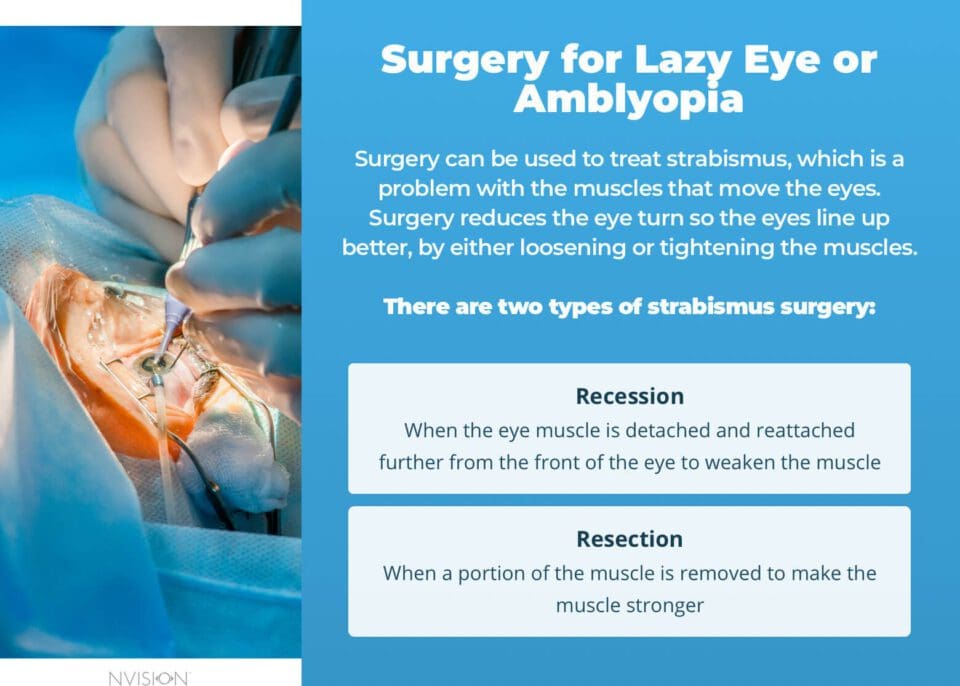
Although an optometrist or ophthalmologist will try less invasive treatments first, amblyopia may require surgery to treat strabismus, which is a problem with the muscles that move the eyes. This surgery can be performed in both adults and children. The surgery reduces the eye turn, so the eyes line up better, by either loosening or tightening the muscles as needed. There are two types of strabismus surgery:
- Recession, when the eye muscle is detached and reattached further from the front of the eye to weaken the muscle
- Resection, when a portion of the muscle is removed to make the muscle stronger
About 1.2 million of these types of eye surgeries are performed in the U.S. every year. It is a well-known procedure, as it is the third most common type of eye surgery in the country. Like other eye surgeries, it is a one-day procedure that is outpatient, so your child does not have to stay in the hospital and can return to school after a few days of rest.
This procedure may improve vision, but it is not guaranteed to do so. In some instances, surgery is more cosmetic. However, surgery in concert with nonsurgical treatments like eye patches may reduce the risk of long-term vision loss.
Surgical treatments may also remove corneal ulcers and cataracts, adjust drooping eyelids, or correct other tissue damage from an injury or accident that hurt the eye.
Living With Lazy Eye
People who have lazy eye are unable to blend images together. This means they lack binocular vision and are unable to accurately assess distance. This can result in accidents as people may walk into things. When they reach out to grab something, they may grab next to the object rather than the object itself.
Children learn to adapt to the issue, so they often rely on other clues to assess depth perception.
The effects of lazy eye on quality of life differ between children and adults. For adults dealing with this condition, learning how to fix lazy eyes can lead to enhanced self-esteem and decreased feelings of frustration or shame. Children who have lazy eye are sometimes bullied by peers, resulting in reduced self-esteem.
Lazy eye is also a cosmetic issue. Surgery and other treatments that can correct the issue often improve aesthetics, helping people to feel less self-conscious and gain confidence.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Managing Eyesight
Grown ups struggling with a lazy eye may wonder how to fix lazy eyes in adults. The process of managing eyesight and finding effective treatment requires close collaboration with an eye doctor and adherence to prescribed treatments, including potential surgical procedures.
If you are prescribed eyeglasses or contacts to help the issue, wear these as prescribed.
If your eye doctor recommends patch use, follow their instructions closely. The guidelines of your eye patch use will vary according to the severity of your lazy eye.
Likewise, use eye drops as prescribed. If you don’t use prescribed methods as instructed, you are less likely to see results.
Surgery can give the most dramatic improvement in your eyesight and overall appearance. Follow your eye doctor’s recommendations for pre-op and post-op care.
There is no evidence that eye exercises will improve amblyopia on their own. However, your eye doctor may recommend certain eye exercises in combination with other treatments.
Get regular eye exams, on a schedule recommended by your doctor.
Resources for Families With Visual Impairments
How to Pick a Treatment for Your Child’s Lazy Eye
Your child’s eye doctor will inform you on how serious lazy eye is and if underlying issues like cataract, corneal ulcers, or strabismus are dramatically impacting vision. If the condition is very serious, your child may need surgery. Additionally, if an adult has lazy eye, surgery may improve the appearance overall and could help to regain a little vision. For the most part, however, clinicians will recommend nonsurgical treatments for children, as they are noninvasive.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Amblyopia (Lazy Eye) in Children. (March 2014). CMAJ – JAMC.
- Amblyopia: What Is Lazy Eye? (October 16, 2018). American Academy of Ophthalmology (AAO).
- Amblyopia: Lazy Eye Diagnosis & Treatment. (October 16, 2018). American Academy of Ophthalmology (AAO).
- Lazy Eye Surgery Facts. (March 4, 2017). American Academy of Ophthalmology (AAO).
- Amblyopia. Fighting Blindness.
- Amblyopia and Quality of Life: A Systematic Review. (April 2011). Eye: The Scientific Journal of the Royal College of Ophthalmologists.
- The Effects of Strabismus on Quality of Life in Adults. (November 2007). American Journal of Ophthalmologists.
- Short-Term Deprivation of the Amblyopic Eye, Combined With Physical Exercise, Promotes Long-Term Visual Recovery in Young Amblyopic Children. (July 2019). Investigative Ophthalmology & Visual Science.

Dr. Raoof is a fellowship-trained and board-certified cataract, cornea and LASIK surgeon. She is a highly acclaimed ophthalmologist and influential surgeon in the eye care industry.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

