Guide to Pinguecula (& How to Treat It)
Home / Eye Conditions & Eye Diseases /
Last Updated:
What Is Pinguecula?
A pinguecula is a growth of fat, protein, or calcium on the conjunctiva. They are caused when the eye is exposed to sand, dust, and ultraviolet rays. They are sometimes called surfer’s eye.
Table of Contents
A pinguecula is harmless. It usually only requires eye drops and better protection to dissipate and return the eye’s appearance to normal,
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Some patients might experience discomfort from the growths, so they might be prescribed special contact lenses. Surgery is an option, but it is mostly done for cosmetic purposes. More often than not, basic care will resolve a pinguecula.
Why Is It Called ‘Surfer’s Eye’?
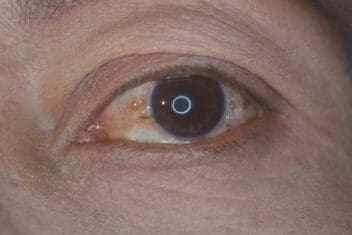
A pinguecula is thought to be caused by a combination of dry eyes and exposure to wind, dust, or ultraviolet light from the sun. Since surfers are continually exposed to these conditions, a pinguecula is sometimes known as surfer’s eye.
The condition is most commonly found among people who live in tropical climates. Any constant irritation to the eye can lead to a pinguecula regardless of location or activity, however.
Symptoms of a Pinguecula
Generally, a pinguecula appears as a small, yellowish growth on the eye. It may look like a small bump.
Symptoms may be very minor to severe, depending on the size of the pinguecula. They include the following:
- Dryness
- Itchiness
- Swelling
- Redness
- Feeling like you have something in your eye
Prevention
There are some simple ways to protect the eye from the most straightforward risk factors for a pinguecula.
- Wear sunglasses to protect the eyes from ultraviolet light.
- Wear glasses or goggles to keep dust out.
- Use artificial tears to lubricate the eyes and help them maintain moisture.
Eye Protection
While wearing protective lenses on sunny days seems obvious, people at risk for a pinguecula — such as those who come into contact with a lot of dust and sand or those who have dry eyes in general — might want to wear sunglasses on cloudy days. The sun’s UV rays can easily penetrate cloud cover, and this can precipitate the formation of a pinguecula even without direct sunlight.
Sunglasses with wraparound frames offer the best protection since regular frames don’t block all the sunlight the eyes can be exposed to.

Another option might be to wear photochromic lenses, which block out 100 percent of ultraviolet radiation. They are designed to protect the eyes from the harmful high-energy blue light by automatically darkening when coming into contact with that level of sunlight.
The beach is not the only place where a person might have enough risk conditions for the formation of pinguecula. ABC News explains that during winter, fresh snow can reflect up to 80 percent of the ultraviolet radiation coming from the sun. People who ski, snowboard, or spend a lot of time in the snow should wear well-fitting ski goggles to avoid snow blindness and to protect their eyes from absorbing enough UV radiation that it causes a pinguecula to grow.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Dry Eyes and Eye Drops
Dry eye disease can also be a contributing factor to the development of a pinguecula. They tend to form in middle-aged or older people who spend a lot of time in the sun, but it is not unheard of for a pinguecula to form in younger adults or even children. Anybody who spends a lot of time in the sun — without wearing sunglasses, hats, goggles, or anything else to protect their eyes — is at risk for developing a pinguecula.
If the pinguecula is advanced enough to cause redness and swelling in the eye (the result of extra blood vessels forming in the conjunctiva), a doctor may recommend steroid eye drops. The eye drops can also help to counter the feeling of a physical object (like dust or sand) in the eye. Surgery is not usually needed for pinguecula, but patients might qualify for surgery if the eye drops take too long to work or if they need immediate relief.
Pinguecula Surgery
It is very rare for a pinguecula to require surgery. Most often, steroid eye drops can be used to effectively treat the issue.
In severe cases, however, a pinguecula can be so large that it affects vision, or it may be a cosmetic issue. When these cases don’t respond to eye drops, surgery may be recommended.
Surgery to remove a pinguecula is a simple outpatient procedure, and the recovery process is straightforward. The pinguecula is carefully cut away from the eye. The surgeon will usually place a tissue graft over the removal site, in order to prevent future regrowth.
Pingueculitis and Scleral Contact Lenses
In particularly bad cases, the pinguecula can become inflamed and swollen, leading to a condition known as pingueculitis. American Family Physician explains that pinguecula treatment can include artificial tears and mild topical steroids if necessary. This should cause the swelling to recede, and it might remove the pinguecula entirely; however, if the patient does not want to wait, surgery is an option.
Additionally, if pinguecula or pingueculitis causes chronic irritation, or the pinguecula interferes with contact lenses, surgery might be a consideration.
Another pinguecula treatment option is scleral contact lenses. They cover both the cornea and a large part of the sclera (the white part of the eye). This helps to protect the growth from further exposure to UV rays. This will break up the protein, fat, or calcium deposit and cause the pinguecula to dissipate.
This might be an option for people whose pinguecula interferes with the application of their regular contact lenses since scleral contact lenses “completely vault the cornea,” bypassing the problems posed by an irregular corneal surface.
People who have a pinguecula experience an itching and burning sensation in their eyes, like feeling like they have sand or grit caught on their eye. This might be how the pinguecula started, but it is not actually pinguecula itself. The formation of the pinguecula can make their vision blurry.
Pinguecula vs. Pterygia

Occasionally, a pinguecula is confused with another form of eye growth called a pterygia. Sometimes the two are mentioned together, but they are distinct conditions.
A pterygia is the growth of fleshy tissue that can start as a pinguecula, but it grows large enough to cover the cornea and affect vision. A pinguecula does not grow, does not cover the cornea, and does not affect vision.
The causes for both a pterygium and a pinguecula are the same (exposure to the sun’s UV rays, exposure to sand, and dry eyes), but their respective developments and prognoses are different. In 1979, a study of people with pinguecula who live in the Arctic Circle clarified that a pinguecula and a pterygium are “two different disorders.”
What Should I Do About Pinguecula?
Despite the discomfort and distress of seeing an unusual growth on the eye, a pinguecula is noncancerous and generally not a cause for concern. Pinguecula treatment is generally simple and lifestyle changes can help return the eye to its normal appearance.
There are rarely any long-term consequences of a pinguecula. They have been known to grow back after surgery, especially if the patient continues to expose their eyes to dust, sand, and UV rays.
A pinguecula is benign, but if it changes in size, shape, or color, or if it causes significant itching or burning to the eyes (beyond what is to be expected from pinguecula), a patient should report this to their doctor immediately.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Pinguecula. ScienceDirect.
- Six Things to Know About Pinguecula and Pterygium. (July 28, 2016). American Academy of Ophthalmology.
- Artificial Tears: How to Select Eye Drops for Your Eyes. (February 11, 2016). Mayo Clinic.
- Why You Should Be Wearing Sunglasses in the Winter. (January 29, 2019). ABC News.
- Everything You Need to Know About Snow Blindness. (October 18, 2018). Healthline.
- Acute Red Eye. (September 15, 2007). American Family Physician.
- Getting Creative With Scleral Lenses: Part 1. (January 25, 2012). Review of Cornea & Contact Lenses.
- What Is a Pinguecula and a Pterygium (Surfer’s Eye)? (September 1, 2017). American Academy of Ophthalmology.
- Prevalence of Pinguecula in Greenland and in Copenhagen, and Its Relation to Pterygium and Spheroid Degeneration. (February 1979). Acta Ophthalmologica .
- Pinguecula. (November 21, 2017). Healthline.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.

