The Connection Between Diabetes and Vision
Home /
Last Updated:
Diabetes creates high blood sugar (glucose) levels, which causes glucose to collect in the blood. This narrows blood vessels, reducing the flow of blood and oxygen and increasing the risk of damaged vessels.
Table of Contents
The rise and fall of blood sugar, and the damage to small blood vessels, can cause vision and eye health problems.
The most common short-term effect of diabetes on vision and eye health is blurry vision, caused by swelling or reduced brain function due to the rise and fall of blood sugar levels in the body.
Continually high levels of glucose in the blood over an extended period of time can cause damage to the small blood vessels behind the eyes due to the narrowing of blood vessels and lack of blood and oxygen flow. This is the cause of the most serious diabetes-related eye problems.
Diabetic retinopathy is a diabetic eye disease that causes blood cells in the retina to bleed or hemorrhage. It develops through four stages, and it is the most common cause of blindness for those with diabetes.
Diabetic macular edema (DME) is a result of diabetic retinopathy. It causes fluid buildup in part of the retina.
Those with diabetes are more likely to develop cataracts, a condition that causes clouding of the eye’s lens.

People with diabetes are also about twice as likely to develop glaucoma, a group of diseases that damage the eye’s optic nerve.
Because many diabetic eye diseases have few symptoms, and they are much more treatable in their early stages, thorough annual eye exams are key in preventing diabetic eye damage. Proper diabetes management, along with a healthy diet containing certain nutrients, can also prevent disease and promote eye health.
The Link Between Diabetes and Vision Problems
Glucose comes from food, and it is a vital source of energy for the body. Insulin is a hormone (a chemical messenger in the body) that controls glucose, transforming it into fuel.
Diabetes causes people to have high levels of blood sugar.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
It’s the result of either having too much or not enough insulin. This is type 1 diabetes, which makes up approximately 5 percent of people with diabetes.
It can also be the result of not being able to properly use the insulin being produced. This is type 2 diabetes, which makes up 90 to 95 percent of people with diabetes.
Both types of diabetes cause the body to be unable to store and use glucose. Instead of reaching the cells that need it, glucose collects in the blood, reducing the elasticity of blood cells. This causes the blood vessels to narrow and inhibits blood flow.
The reduced supply of oxygen and blood increases the risk of high blood pressure and damage to both the small blood vessels (microvascular disease) and large blood vessels (macrovascular disease).
Most eye and vision-related diabetes complications are the result of rising and falling blood sugar levels in the body or due to microvascular disease.
Diabetes and Vision: Short-Term Effects

The most common effect of diabetes on short-term vision and eye health is blurry vision. When someone has blurry vision, things may appear out of focus. They may be unable to see details or feel that things look fuzzy. The blurriness may be mild or extremely noticeable.
Blurry vision may be a symptom of long-term diabetes complications or an indication of a more serious problem. When experienced as a short-term side effect of diabetes, blurry vision is the result of rising and falling blood sugar levels.
This type of blurred vision can occur due to:
- Swelling. High glucose levels can cause fluid to move into and out of the eye, irritating the eye lens and causing it to swell. The swelling changes the shape of the eye, which causes blurriness, as the lens plays an important role in light reflection and vision.
- Hypoglycemia. A crash in glucose can lead to low blood sugar, or hypoglycemia. This can have a negative impact on brain function, which can cause blurred vision.
Both of the above conditions are short-term issues. Vision will return to normal (non-blurry) after blood sugar levels normalize. Short-term blurred vision is very unlikely to cause vision loss.
Long-Term Effects of Diabetes: Blood Vessel Damage
Eye and vision complications from diabetes are progressive. If left untreated, they get worse with time.
Continually high levels of glucose in the blood over an extended period of time can cause damage to the small blood vessels behind the eyes due to the narrowing of blood vessels and lack of blood and oxygen flow. This damage can even begin in prediabetes — a condition in which a person has consistently high blood sugar levels but has not yet fully developed type 2 diabetes.
Damaged blood vessels behind and near the eye can result in swelling and fluid leakage. New blood vessels may develop and ultimately begin to bleed in parts of the eye. These weaker new blood vessels may cause scarring or high blood pressure inside the eye.
Most serious diabetes-related eye and vision problems are caused by issues relating to blood vessel damage, including the most common diabetic eye diseases.
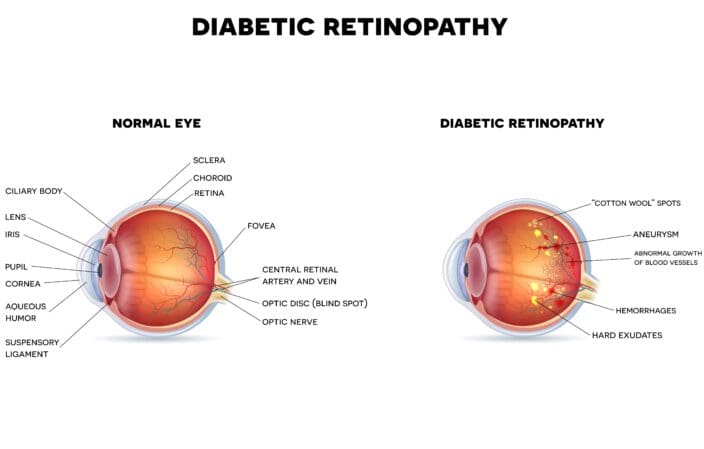
Diabetic Retinopathy
As the inner lining in the back of each eye, the retina senses light and transmits it to the brain via the optic nerve. Diabetic retinopathy causes blood cells in the retina to leak or hemorrhage.
The disease progresses through four stages.
- Mild nonproliferative retinopathy: At this earliest stage, tiny areas of swelling occur in the small blood vessels of the retina. These swellings, called microaneurysms, may cause distorted vision by oozing fluid into the retina.
- Moderate nonproliferative retinopathy: As the issue worsens, two conditions characterize this progressive phase. The blood vessels whose job it is to provide nourishment to the retina may begin to distort and swell. These vessels may also become unable to move blood. These conditions may change how the retina looks and may cause diabetic macular edema (DME).
- Severe nonproliferative retinopathy: Additional blood vessels are jammed as the disease advances. Areas of the retina are deprived of blood; they tell the retina to produce new blood vessels.
- Proliferative diabetic retinopathy (PDR): This is the most advanced stage of the disease. The blood-deprived areas of the retina have already sent signals to grow new blood vessels. These weak new blood vessels are along the inside of the retina and into the vitreous gel. The fragile new vessels may leak and eventually bleed. Associated scar tissue may contract, causing retinal detachment as the contracting scar tissues pulls the retina with it, tearing it from the underlying tissue. This detachment can trigger irreversible vision loss.
Among people with diabetes, diabetic retinopathy is the most common cause of blindness. It’s also the leading cause of vision impairment and vision loss among working-age adults.
The early stages of diabetic retinopathy may have no symptoms, which can make the disease hard to notice until it’s more advanced and affecting vision. Sometimes abnormal vessels may bleed and cause “spots,” which may clear on their own but will lead to more bleeding if not treated.
If vision is lost due to diabetic retinopathy, it may be irreversible. However, controlling diabetes and maintaining normal blood pressure and cholesterol slow the onset and development of diabetic retinopathy.
Treatment for diabetic retinopathy is sometimes delayed until an individual develops PDR or DME. PDR is usually treated with panretinal laser surgery or a vitrectomy, the removal of the vitreous gel in the center of the eye.
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
Diabetic Macular Edema (DME)
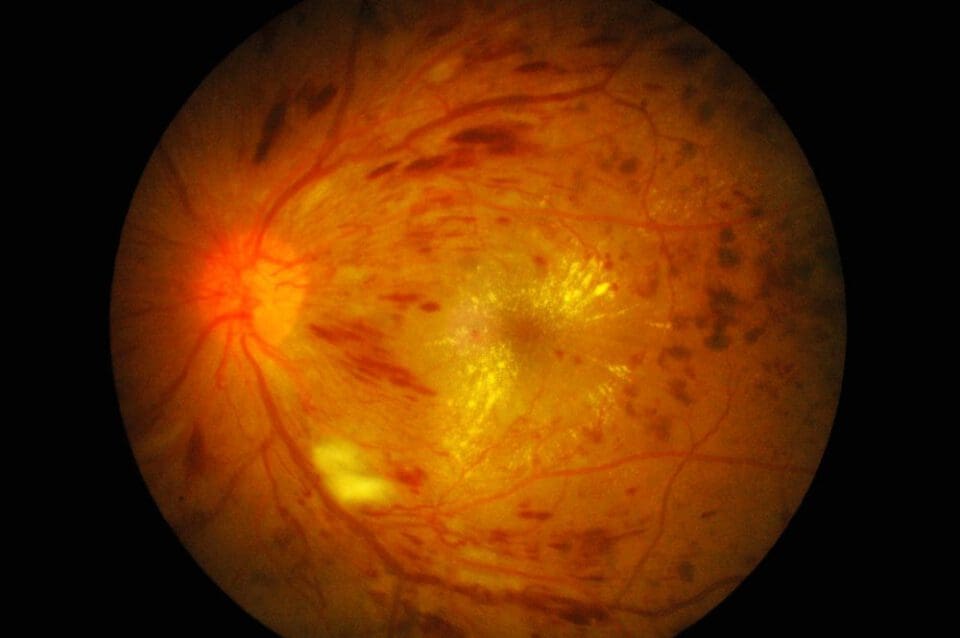
Although most commonly seen in those suffering from advanced diabetic retinopathy, this macula buildup can occur at any stage of the disease. DME occurs in about half of all people who have diabetic retinopathy. It’s the most common cause of vision loss among people with have diabetic retinopathy.
DME is often treated with focal/grid macular surgery in conjunction with DME-suppressing corticosteroids or with anti-VEGF, which stops the growth of new blood vessels by blocking a protein called vascular endothelial growth factor (VEGF)
Cataracts
Adults with diabetes are about two to five times more likely to develop cataracts, a clouding of the eye’s lens, than those without diabetes. Adults with diabetes are also likely to develop a cataract at an earlier age.
Cataracts as a result of other health problems, such as diabetes, are called secondary cataracts.
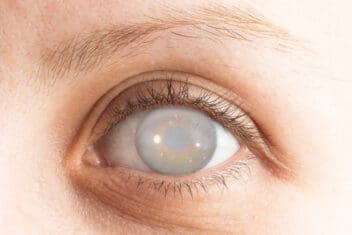
Symptoms of cataract include:
- Cloudy, blurred, or faded vision.
- Excessive glare or a “halo” around lights.
- Poor night vision.
- Frequent changes in prescriptions.
- Double vision.
Early symptoms of cataracts may be treated with new eyeglasses, brighter lighting, and magnifying glasses.
If the disease is caught too late or the symptoms are not helped, surgery may be necessary. In surgery, the cloudy lens is removed and replaced with an artificial lens.
Glaucoma
Adults with diabetes are approximately twice as likely to develop glaucoma than adults without diabetes. Sometimes associated with increased blood pressure or pressure inside the eye, glaucoma is a group of diseases that harm the eye’s optic nerve — a cluster of nerve cells that connect the eye to the brain.
The early stages of glaucoma have no symptoms. Glaucoma can develop in one or both eyes without the person feeling any pain or noticing any vision changes.
Untreated, glaucoma will cause the individual to lose side (peripheral) vision, and they may not see things off to the side or in the corner of their eye. Eventually, straight-ahead (central) vision will also be decreased until vision is lost.
There is no cure for glaucoma, and vision lost from it is irreversible. However, in the early stages of glaucoma, treatments can significantly slow its development. The sooner the glaucoma is caught, the more effective treatment can be.
Treatments include medication, which may lower eye blood pressure, and laser or conventional surgery
Preventing Diabetic Eye Damage

Most of the leading diabetic eye diseases have subtle symptoms in their early stages or no symptoms at all. All of them are far easier to treat in the early stages before advanced development or irreversible vision loss.
This is why it’s so important for individuals with diabetes to get thorough eye exams with a diabetes-experienced ophthalmologist annually. People who already have a diabetic eye disease or are at a high risk for developing one may need to go more frequently.
Proper management of diabetes is very important in preventing diabetic eye damage. Symptoms of out-of-control diabetes, such as continually high blood sugar or blood pressure, can lead to the development or worsening of diabetic eye diseases and eye damage. Effectively managing diabetes symptoms can relieve both the short-term and long-term effects of diabetic eye health and vision, especially in the early stages of a condition.
Finally, a healthy lifestyle and diet can help to better control diabetes and to improve eye health and function. A balanced amount of exercise and sleep may help an individual to maintain healthy blood sugar and blood pressure, while a diet of unprocessed, nourishing foods can help to boost eye health.
Certain foods contain vitamins and minerals known to improve eye health. These include leafy greens like spinach and kale (vitamin C and phytochemicals), eggs (omega-3 acids, lutein, and vitamin E), and nuts (zinc, vitamin E, and omega-3s).
You deserve clear vision. We can help.
With 135+ locations and over 2.5 million procedures performed, our board-certified eye surgeons deliver results you can trust.
Your journey to better vision starts here.
References
- Effects of Diabetes on the Body and Organs. (April 29, 2019). Medical News Today.
- Diabetes: The Differences Between Types 1 and 2. (March 25, 2019). Medical News Today.
- What Is the Link Between Blurry Vision and Diabetes? (December 12, 2018). Medical News Today.
- Diabetic Eye Disease. (May 2017). National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
- Facts About Diabetic Eye Disease. (September 2015). National Eye Institute (NEI).
- Facts About Cataract. (September 2015). National Eye Institute (NEI).
- Facts About Glaucoma. (September 2015). National Eye Institute (NEI).
- Top 10 Foods for Healthy Eyes. (March 17, 2018). Medical News Today.
This content is for informational purposes only. It may have been reviewed by a licensed physician, but is not intended to serve as a substitute for professional medical advice. Always consult your healthcare provider with any health concerns. For more, read our Privacy Policy and Editorial Policy.
